What Is Knee Ligament Surgery? Types, Procedure & Recovery

What Is Knee Ligament Surgery? Types, Procedure & Recovery Knee ligament surgery is a specialized orthopedic procedure performed to repair or reconstruct damaged ligaments in the knee joint. Knee ligament injuries are common among athletes, active individuals, and even older adults due to accidents, sports injuries, or degenerative changes. When non-surgical treatment fails, knee ligament surgery becomes essential to restore knee stability, strength, and normal movement. Understanding knee ligaments, their function, types of injuries, and recovery after knee ligament surgery helps patients make informed decisions and achieve better long-term outcomes. What Is Knee Ligament Surgery? Knee ligament surgery is performed to repair or reconstruct torn or severely damaged knee ligaments. In most cases, surgeons reconstruct the ligament using a graft rather than stitching the torn ligament directly. This surgery is commonly recommended when a knee ligament tear leads to: Chronic knee instability Repeated knee giving way Inability to return to sports or daily activities Failure of conservative knee ligament injury treatment Modern knee ligament surgery is usually done using minimally invasive arthroscopic techniques, ensuring faster recovery and reduced pain. What Are Knee Ligaments and Why Are They Important? The knee joint is one of the most complex joints in the human body. It depends heavily on the knee ligaments to maintain stability and proper movement. Knee joint ligaments connect bones to bones and prevent excessive movement that could damage the joint. The four main knee ligaments include: Anterior Cruciate Ligament (ACL) – Controls forward movement of the shin bone Posterior Cruciate Ligament (PCL) – Prevents backward movement of the shin bone Medial Collateral Ligament (MCL) – Provides inner knee stability Lateral Collateral Ligament (LCL) – Stabilizes the outer knee Damage to any of these knee joint ligaments can cause pain, swelling, instability, and difficulty walking or playing sports. Types of Knee Ligament Surgery Different types of knee ligament surgery are performed based on the specific ligament injured. ACL Knee Ligament Surgery ACL reconstruction is the most common knee ligament surgery, especially in athletes. Uses tendon grafts from hamstring, patellar, or donor tissue Restores knee stability during twisting movements Prevents long-term joint damage PCL Knee Ligament Surgery PCL injuries may require surgery when instability persists. Usually performed for severe ligament tears Helps regain knee strength and function MCL Knee Ligament Surgery Most MCL injuries heal without surgery, but surgery is required when: There is a complete knee ligament tear Multiple ligaments are damaged LCL Knee Ligament Surgery LCL injuries often occur with other ligament injuries and require surgical repair for stability. Causes of Knee Ligament Tear A knee ligament tear occurs due to sudden injury or repeated stress on the knee. It is commonly caused by sports activities, sudden twisting movements, direct impact, falls, or accidents, leading to pain, swelling, instability, and difficulty in normal knee movement. Sports injuries (football, cricket, basketball, skiing) Sudden twisting or pivoting movements Direct blow to the knee Road traffic accidents Falls or missteps Degenerative weakening of the knee ligaments Knee Ligament Tear Symptoms Recognizing knee ligament tear symptoms early is important to avoid further damage. Common symptoms include sudden knee pain, swelling, stiffness, instability, difficulty walking, reduced movement, and a popping sensation at the time of injury, especially during sports or sudden twisting activities. Common symptoms include: Sudden knee pain Swelling within hours of injury Knee instability or “giving way” Difficulty walking or running Reduced range of motion Popping sensation at the time of injury Persistent knee ligament tear symptoms often indicate the need for advanced knee ligament injury treatment or surgery. Diagnosis Before Knee Ligament Surgery Accurate diagnosis is crucial before performing knee ligament surgery. Doctors use a combination of: Physical examination X-rays (to rule out fractures) MRI scans (gold standard for knee ligament injuries) MRI helps visualize knee joint ligaments clearly and determine the severity of the tear. Procedure of Knee Ligament Surgery Modern knee ligament surgery is typically performed arthroscopically. Step-by-Step Knee Ligament Surgery Procedure Anesthesia – General or spinal anesthesia is given Arthroscopic Evaluation – Small incisions are made to insert a camera Removal of Torn Ligament – Damaged tissue is cleared Graft Placement – New ligament graft is positioned Fixation – Graft is secured with screws or anchors Closure – Incisions are closed with minimal scarring This minimally invasive approach reduces pain and speeds up recovery after knee ligament surgery. Knee Ligament Injury Treatment: Surgery vs Non-Surgical Care Not every knee injury needs surgery. Knee ligament injury treatment depends on the severity of the tear, knee stability, and the patient’s activity level. Mild injuries often heal with rest and physiotherapy, while severe or unstable ligament tears may require surgical treatment for full recovery. Non-Surgical Treatment Options Rest and activity modification Knee braces Physiotherapy Pain management When Knee Ligament Surgery Is Recommended Complete ligament tear Persistent instability Failure of conservative treatment Athletes want full performance recovery Recovery After Knee Ligament Surgery Recovery plays a vital role in the success of knee ligament surgery. Proper physiotherapy, guided exercises, and gradual activity progression help restore strength, flexibility, and stability of the knee, reduce complications, and ensure a safe return to daily activities and sports over time. Recovery Timeline Week 1–2: Pain control and swelling reduction Weeks 3–6: Regaining knee motion and strength Months 3–6: Advanced strengthening and balance training 6–9 Months: Return to sports activities Physiotherapy After Knee Ligament Surgery Physiotherapy focuses on: Strengthening muscles around the knee Improving balance and coordination Protecting healing knee ligaments Skipping rehab can compromise surgical results. Benefits of Knee Ligament Surgery Successful knee ligament surgery helps restore knee stability, reduce long-term pain, and improve mobility. It allows patients to return to daily activities and sports safely, prevents further joint damage, and enhances overall knee strength and confidence with proper rehabilitation and care. Restores knee stability Reduces chronic pain Prevents further joint damage Improves mobility and confidence Allows safe return to sports and an active lifestyle Risks and Complications of Knee Ligament Surgery Although safe, knee ligament surgery may involve some risks: Infection Stiffness Blood clots
Bad Signs After ACL Surgery: Warning Symptoms You Shouldn’t Ignore
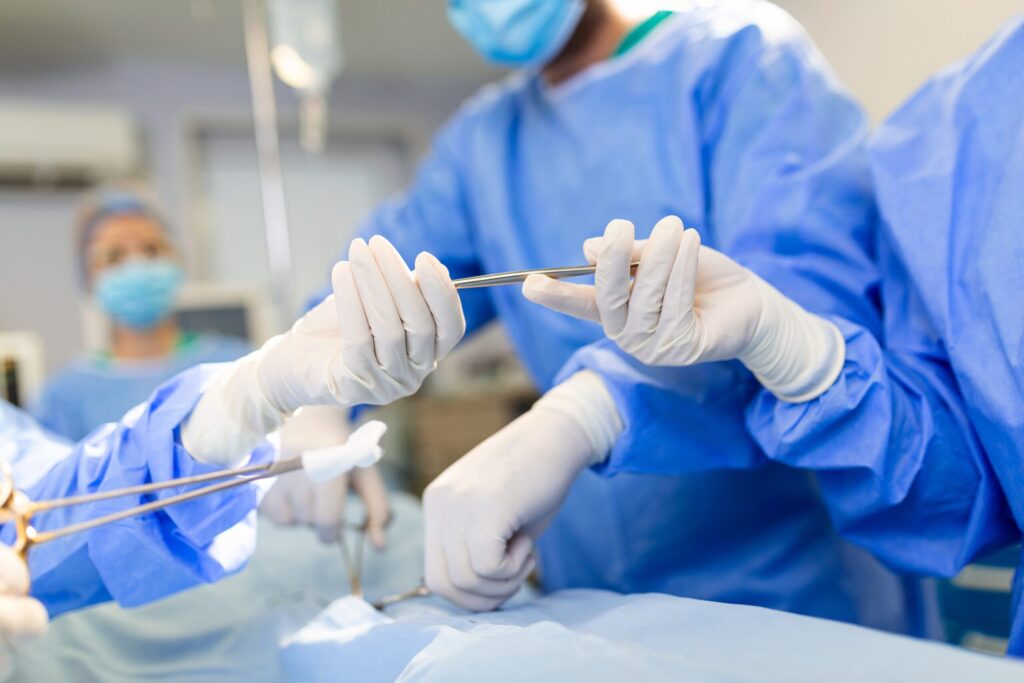
Bad Signs After ACL Surgery: Warning Symptoms You Shouldn’t Ignore ACL surgery is often a turning point for people dealing with serious knee injuries. It promises stability, strength, and a return to normal movement. However, recovery is not always smooth for everyone. While some discomfort is part of healing, certain symptoms may signal deeper problems. These Bad Signs After ACL Surgery should never be ignored because they can affect long-term knee function if left unaddressed. Many patients feel unsure about what is normal after surgery and what is not. This confusion often leads to delays in identifying complications. In this detailed guide, we will break down what to expect after ACL surgery, common warning signs, recovery challenges, and how to understand your body better during healing. Knowing these signs early can protect your knee and support a safer recovery journey. What is ACL surgery and the Recovery Process ACL surgery is performed to repair or reconstruct the anterior cruciate ligament, which is crucial for knee stability. This ligament helps control twisting, pivoting, and sudden movements. Injuries often occur during sports, falls, or accidents. After ACL surgery, the body begins healing in phases. Common experiences include: Swelling around the knee joint Pain or soreness, especially in the first few weeks Stiffness and reduced range of motion Weakness in the thigh muscles These symptoms usually improve gradually with physiotherapy and rest. However, Bad Signs After ACL Surgery appear when recovery stalls or symptoms worsen instead of improving. Recognizing this difference early is essential. Pain After ACL Surgery: When Normal Turns Into a Warning Pain is expected after surgery, but pain after ACL surgery should slowly decrease with time. One of the most common Bad Signs After ACL Surgery is pain that increases instead of settling down. Pain becomes concerning when: It feels sharp, stabbing, or deep inside the knee It worsens at night or disrupts sleep It increases during simple activities like walking It does not improve despite rest and exercises Mild discomfort during physiotherapy is normal. However, constant or worsening pain may interfere with rehabilitation and extend ACL surgery recovery time. Listening to pain signals helps prevent further complications. Swelling That Refuses to Go Away Swelling is a natural response after surgery, but persistent swelling is one of the clear Bad Signs After ACL Surgery. Normal swelling: Reduces gradually over weeks Improves with rest, elevation, and exercise Abnormal swelling may include: Knee remaining visibly swollen for long periods Tight or heavy sensation in the joint Difficulty bending or straightening the knee Warmth around the knee that does not subside When swelling and stiffness occur together, they can restrict movement and slow recovery. Managing swelling early helps prevent long-term joint stiffness. Delayed ACL Surgery Recovery Time and Limited Mobility Regaining knee movement is a major goal after surgery. One of the concerning Bad Signs After ACL Surgery is delayed progress in movement and flexibility. Signs of delayed recovery include: Difficulty fully straightening the knee Limited bending even after weeks of therapy Painful walking or limping No noticeable improvement despite regular physiotherapy A delayed ACL surgery recovery time can affect muscle strength, balance, and confidence. Early attention to limited mobility can prevent permanent restrictions and support better outcomes. Knee Instability and the “Giving Way” Feeling A feeling of instability is one of the most serious Bad Signs After ACL Surgery. The surgery aims to restore knee stability, so ongoing instability is not normal. Warning signs include: Knee buckling during walking Sudden loss of balance Fear of putting weight on the leg Difficulty turning or changing direction This sensation can increase the risk of re-injury and affect daily activities. During early recovery, support tools like a Knee Brace for ACL Injuries can help improve confidence, but persistent instability should always be addressed. Infection-Related Symptoms You Should Watch For Although uncommon, infection-related symptoms are important Bad Signs After ACL Surgery and should not be overlooked. Possible warning signs include: Increasing redness around the incision Unusual fluid discharge Foul smell from the surgical site Persistent warmth or tenderness While mild tenderness is expected, worsening symptoms over time may delay healing and prolong recovery. Paying attention to incision changes is a key part of recovery awareness. Challenges After ACL and Meniscus Surgery Some patients undergo ACL and meniscus surgery together. This combined procedure often requires more careful rehabilitation. Recovery challenges may include: Slower improvement in movement Increased stiffness Joint locking or clicking sensations Uneven pain distribution While a slightly longer recovery is normal, worsening symptoms may become Bad Signs After ACL Surgery if ignored. Understanding these challenges helps patients set realistic expectations and respond early. Emotional and Mental Signs That Affect Recovery Recovery is not just physical. Emotional changes can also be subtle Bad Signs After ACL Surgery. Common emotional challenges include: Fear of re-injury Frustration with slow progress Loss of confidence in knee strength Anxiety about returning to sports or work Mental stress can indirectly slow physical recovery. Staying informed and patient-focused during ACL Injury & Reconstruction Surgery recovery helps maintain motivation and consistency. Exploring Treatment Options and Cost Awareness When recovery does not go as planned, timely adjustments make a big difference. Important considerations include: Physiotherapy modifications Supportive braces or aids Follow-up assessments Understanding acl surgery cost is also important for long-term planning. Costs may vary depending on treatment needs, rehabilitation duration, and follow-up care. Some individuals explore acl tear treatment without surgery for partial tears, but post-surgical symptoms should never be ignored. Early care often reduces long-term expenses and recovery time. Normal Healing vs Bad Signs After ACL Surgery Recovery Aspect Normal Healing Bad Signs After ACL Surgery Pain Gradually decreases Becomes severe or constant Swelling Reduces over time Persists or worsens Movement Improves steadily Remains restricted Stability Knee feels secure The knee gives way Recovery Time On track Delayed progress Long-Term Effects of Ignoring Warning Signs Ignoring Bad Signs After ACL Surgery can lead to: Chronic knee pain Reduced flexibility Muscle weakness Difficulty returning to sports or work Delays in addressing
Shoulder Pain Exercises for Fast Recovery, Flexibility, and Joint Strength

Shoulder Pain Exercises for Fast Recovery, Flexibility, and Joint Strength Shoulder pain can significantly affect daily activities, work performance, and overall quality of life. From difficulty lifting objects to discomfort while sleeping, shoulder problems are increasingly common due to poor posture, repetitive movements, sports injuries, and aging. The good news is that shoulder pain exercises play a crucial role in reducing pain, restoring flexibility, and strengthening the shoulder joint for long-term relief. This comprehensive guide explains shoulder pain causes, effective shoulder pain exercises, treatment approaches, and recovery tips to help you regain pain-free movement safely and efficiently. Understanding Shoulder Pain and Its Impact on Daily Life The shoulder is one of the most mobile joints in the body, making it more vulnerable to injury and strain. Shoulder joint pain can occur suddenly due to trauma or gradually due to overuse and degeneration. Common symptoms include: Pain during arm movement Stiffness or reduced range of motion Weakness in the arm Pain radiating to the neck or upper arm Difficulty performing overhead activities Conditions such as left side shoulder pain, left hand shoulder pain, and chronic shoulder pain often worsen when ignored or treated incorrectly. Causes of Shoulder Pain You Should Not Ignore Understanding the causes of shoulder pain is essential before starting shoulder pain exercises because different conditions require different treatment approaches. Shoulder pain may result from muscle strain, ligament injury, joint degeneration, or nerve-related issues. Identifying the exact cause helps in selecting the right exercises, avoiding movements that may worsen the condition, and ensuring faster, safer recovery. Without proper diagnosis, incorrect exercises can increase inflammation, prolong pain, or lead to chronic shoulder problems. Shoulder Pain Causes Related to Injury Rotator cuff tears Shoulder dislocation Sports-related injuries Falls or accidents Overuse injuries Medical and Lifestyle-Related Causes of Shoulder Pain Frozen shoulder Arthritis Tendinitis or bursitis Poor posture Repetitive strain Both left-sided shoulder pain and shoulder injury pain can develop due to improper movement patterns and lack of shoulder strength. Why Shoulder Pain Exercises Are Essential for Recovery Shoulder pain exercises are a cornerstone of non-surgical treatment and rehabilitation. When performed correctly, these exercises help: Reduce inflammation and stiffness Improve flexibility and joint mobility Strengthen shoulder muscles Enhance blood circulation Prevent recurrence of shoulder pain Unlike medication that offers temporary relief, shoulder pain exercises address the root cause of pain and promote long-term healing. When to Start Shoulder Pain Exercises You can begin shoulder pain exercises when: Acute pain and swelling have reduced A doctor or physiotherapist confirms it is safe Pain does not worsen with gentle movement For chronic shoulder pain, exercises are often introduced gradually and adjusted based on pain tolerance. Best Shoulder Pain Exercises for Flexibility and Mobility 1. Pendulum Exercise for Shoulder Pain Relief This is one of the safest shoulder pain exercises, especially during early recovery. How to perform: Bend forward slightly, letting the affected arm hang down Gently swing the arm in small circles Perform clockwise and counterclockwise movements Benefits: Relieves stiffness Improves joint lubrication Reduces shoulder joint pain 2. Cross-Body Shoulder Stretch Helpful for left hand shoulder pain. How to perform: Bring the affected arm across your chest Use the opposite hand to gently pull it closer Hold for 20–30 seconds Benefits: Improves flexibility Reduces muscle tightness Enhances shoulder pain relief Strengthening Shoulder Pain Exercises for Joint Stability 1. Wall Push-Ups One of the safest strengthening shoulder pain exercises. How to perform: Stand facing a wall Place your hands on the wall at shoulder height Slowly bend your elbows and push back Benefits: Builds shoulder stability Strengthens surrounding muscles Supports shoulder pain treatment 2. Resistance Band External Rotation Ideal for rotator cuff strengthening and shoulder injury pain recovery. How to perform: Hold a resistance band with your elbow bent at 90 degrees Rotate the arm outward slowly Repeat 10–15 times Benefits: Improves shoulder joint strength Prevents future injuries Supports long-term recovery Advanced Shoulder Pain Exercises for Chronic Conditions For individuals suffering from Shoulder Ligament Injury, advanced exercises should be performed under professional supervision. 1. Shoulder Blade Squeeze This exercise targets posture-related shoulder pain causes. How to perform: Sit or stand upright Squeeze shoulder blades together Hold for 5 seconds Benefits: Improves posture Reduces muscle imbalance Decreases shoulder joint pain 2. Overhead Arm Stretch Effective for stiffness and frozen shoulder. How to perform: Raise the affected arm overhead Use the other hand to assist gently Hold for 15–20 seconds Benefits: Enhances flexibility Reduces movement-related pain Improves range of motion Role of Shoulder Pain Exercises in Shoulder Pain Treatment Modern shoulder pain treatment emphasizes conservative care before surgery. Shoulder pain exercises are often combined with: Physiotherapy Heat or cold therapy Pain management techniques Posture correction Activity modification This holistic approach ensures safe and sustainable recovery. Tips to Maximize Results from Shoulder Pain Exercises To get the best outcomes from shoulder pain exercises, follow these guidelines: Perform exercises slowly and with control Avoid movements that increase pain Maintain proper posture Be consistent with your routine Combine exercises with rest and recovery Ignoring pain signals can worsen shoulder injury pain and delay healing. Preventing Shoulder Pain with Regular Exercises Prevention is as important as treatment. Regular shoulder pain exercises help: Strengthen shoulder muscles Improve joint stability Prevent recurring injuries Reduce the risk of chronic shoulder pain People with desk jobs, athletes, and older adults benefit greatly from preventive shoulder exercises. When to Seek Medical Help for Shoulder Pain Consult a specialist if: Pain persists for more than two weeks Movement becomes severely restricted Pain radiates down the arm You experience weakness or numbness Professional guidance ensures the safe progression of shoulder pain exercises and effective treatment. FAQs Are shoulder pain exercises safe for everyone? Yes, shoulder pain exercises are generally safe when performed correctly. However, individuals with severe pain, recent injury, or surgery should consult a specialist before starting. How often should I do shoulder pain exercises? Most shoulder pain exercises can be done 1–2 times daily. Consistency is more important than intensity for
Knock Knees Exercises to Reduce Pain and Correct Knee Position

Knock Knees Exercises to Reduce Pain and Correct Knee Position If you are struggling with misaligned knees, performing the right Knock Knees Exercises can significantly help you in reducing pain, improving alignment, and preventing long-term complications. Knock knees, medically referred to as genu valgum, is a problem that affects children, teenagers, and adults. Left untreated, misaligned knees can place extra stress on your joints and even contribute to a knee ligament injury. This blog will guide you through effective exercises, assessments, and treatment options to naturally correct knock knees and protect your knee health. This comprehensive guide will help you understand how to check knock knees, explore effective exercises, and provide insights into knock knees treatment, including braces and surgical options when necessary. What Are Knock Knees? Knock knees occur when the knees angle inward and touch each other while the ankles remain apart. This can affect your posture, walking gait, and overall leg alignment. In adults, knock knees are often associated with weak hip muscles, improper posture, or obesity, whereas in children, they may be a normal stage of growth. Key indicators of knock knees include: Knees that touch while standing upright Ankles that remain apart Uneven gait or difficulty walking Knee, hip, or lower back discomfort Untreated knock knees may lead to early knee arthritis or chronic pain. That’s why early knock knees treatment and corrective exercises are vital for long-term knee health. How to Check Knock Knees at Home Understanding how to check knock knees at home is simple but important. A home assessment can help determine if a professional evaluation is needed. Steps to Check: Stand upright with your back against a wall Place your knees together naturally Measure the gap between your ankles If the ankle gap exceeds 5–6 cm, it may indicate knock knees. However, a professional orthopedic assessment is recommended for accurate diagnosis. Early detection allows for effective ways to fix knock knees, including exercises and braces. Causes of Knock Knee Problem The root cause of knock knee problem determines the treatment approach. Common causes include: Muscle weakness: Particularly in the hips and thighs Postural issues: Poor walking or sitting habits Nutritional deficiencies: Lack of calcium or vitamin D Obesity: Extra load on knee joints Injury or arthritis: Past trauma or joint degeneration Genetic factors: Family history of knee deformities Identifying the underlying cause helps target knock knees treatment, whether through exercises, lifestyle adjustments, or surgery. Is Knock Knee Curable? Many people ask, is knock knee curable? The answer depends on the severity and age. Children: Mild cases often self-correct with growth. Adults: Muscle-strengthening exercises can improve alignment, reduce pain, and prevent worsening, though structural correction may require medical intervention. In some severe cases, knock knee surgery may be recommended, but most individuals benefit significantly from consistent Knock Knees Exercises and supportive treatments. Role of Knock Knees Exercises in Correction Knock Knees Exercises are essential because they: Strengthen weak muscles (glutes, hips, thighs) Stretch tight inner thighs and calves Improve knee tracking during movement Reduce uneven stress on joints A consistent exercise routine improves knee replacement surgery recovery time and can help prevent future joint problems. Exercises should be performed mindfully and with proper form for maximum benefit. Best Knock Knees Exercises Here are the most effective Knock Knees Exercises for improving alignment and reducing discomfort:a 1. Side-Lying Leg Raises Lie on your side, lift the top leg upward Strengthens outer thighs and hip muscles Helps prevent knees from collapsing inward 2. Clamshell Exercise Lie on your side with knees bent Open your top knee like a clamshell Strengthens glutes and stabilizes the hip 3. Wall Squats with Ball Place a small ball between your knees and squat Builds quadriceps and encourages proper knee tracking Reduces inward knee stress 4. Resistance Band Walks Place a band around your thighs and take sideways steps Improves hip stability and balance Helps fix inward knee motion during walking 5. Inner Thigh Stretch Sit or stand and stretch the inner thigh muscles gently Reduces tension pulling knees inward Essential for posture and alignment Perform these exercises 4–5 times per week. Begin with 10 to 15 reps, and slowly raise the intensity as your strength and comfort improve. How to Fix Knock Knees Naturally To learn how to fix knock knees naturally: Perform daily Knock Knees Exercises Maintain proper posture while walking or sitting Avoid crossing legs for long periods Maintain a healthy body weight Use supportive footwear These simple lifestyle modifications, combined with exercises, often provide significant improvement over time, reducing the need for invasive knock knee surgery. Knee Brace for Knock Knees A knee brace for knock knees can help: Support proper alignment Reduce knee pain during daily activities Increase confidence during exercise While braces do not replace the benefits of strengthening exercises, they are excellent adjuncts, especially in adults or during early rehabilitation after surgery. Knock Knees Treatment Options Knock knees treatment varies based on age, severity, and cause: Non-surgical: Exercises, physical therapy, lifestyle modifications Surgical: Realignment procedures in severe adult cases Supportive devices: Knee braces or orthotic inserts Combining these treatments ensures optimal correction and functional improvement. Informative Table: Exercises and Benefits Exercise Name Primary Benefit Target Area Side Leg Raise Improves alignment Outer thighs Clamshell Reduces knee collapse Glutes Wall Squat with Ball Knee stability Quadriceps Band Walk Hip control Hip abductors Inner Thigh Stretch Reduces inward pull Adductors This table helps visualize how exercises contribute to correcting knock knees effectively. When Knock Knee Surgery May Be Needed Knock knee surgery is considered if: Deformity is severe or painful Non-surgical methods fail Joint damage or arthritis is present Daily activities are significantly impaired Surgery usually involves realigning the bone to restore proper knee mechanics. Post-surgery recovery also benefits from Knock Knees Exercises for long-term stability. Lifestyle Tips to Support Correction Proper nutrition plays a vital role in supporting knee health and enhancing the results of Knock Knees Exercises. Including knee ligament injury recovery food in your diet helps
Left Shoulder Pain: Causes, Sports Injuries, Symptoms & Treatment
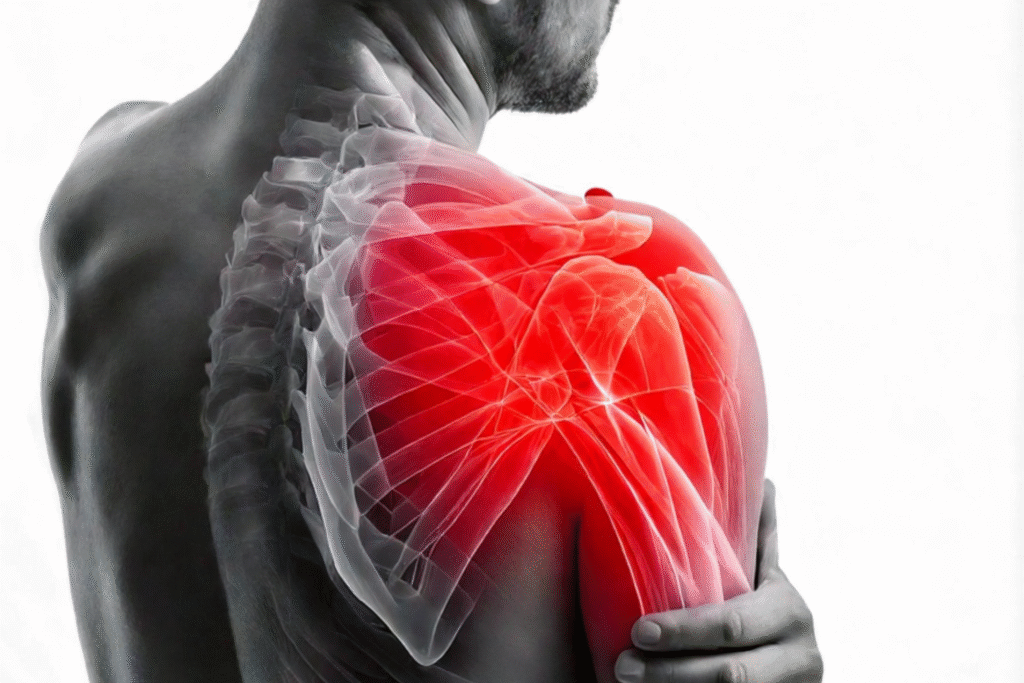
Left Shoulder Pain: Causes, Sports Injuries, Symptoms & Treatment Left shoulder pain is a common problem affecting people of all ages, especially athletes and individuals with active lifestyles. Many cases begin with mild discomfort but gradually worsen due to overuse, poor posture, or untreated sports injuries. In some situations, advanced treatments such as arthroscopic surgery for shoulder pain may be recommended to diagnose and manage internal joint damage accurately. Understanding the causes of shoulder pain, its impact on daily activities, and available treatment options is crucial for effective recovery, improved mobility, and long-term prevention of recurring shoulder problems. Left Shoulder Pain Causes Left shoulder pain can develop due to a wide range of structural and functional issues. The shoulder is a highly mobile joint, making it vulnerable to strain and injury. Everyday movements combined with physical activity often place repeated stress on muscles, tendons, and ligaments. Common causes include: Muscle strain due to overuse or sudden movements Rotator cuff inflammation or tears Shoulder impingement caused by a narrowed joint space Tendonitis or bursitis due to repetitive motion Nerve compression from the neck or upper spine In athletes, left shoulder pain is frequently linked to repetitive overhead actions such as throwing, swimming, or weightlifting. Poor warm-up routines and muscle imbalance further increase injury risk. Over time, untreated shoulder stress can lead to chronic pain, stiffness, and reduced range of motion, making early diagnosis important. Left Shoulder Pain Reasons in Daily Activities Daily habits play a major role in the development of left shoulder pain. Long hours of sitting, incorrect posture, and improper lifting techniques often create continuous stress on the shoulder joint. Even minor movements performed repeatedly can lead to micro-injuries. Key daily-life contributors include: Slouching while working on a computer Sleeping on one side for extended periods Carrying heavy bags on one shoulder Sudden jerky movements while lifting objects Over time, these activities may cause muscle tightness and joint irritation. Left shoulder pain often starts as mild stiffness but can progress to constant discomfort if posture issues are not corrected. Simple lifestyle adjustments such as ergonomic seating, proper sleeping positions, and regular stretching can significantly reduce shoulder strain. Shoulder Injuries in Sports Sports-related injuries are among the leading causes of left shoulder pain. Athletes subject their shoulders to repetitive stress, high-impact forces, and sudden directional changes. This combination makes the joint highly susceptible to injury. Common sports injuries include: Rotator cuff tears in throwing and swimming sports Shoulder subluxation or dislocation in contact sports Labral tears caused by repetitive overhead motion Overuse injuries from excessive training without recovery Inadequate rest and improper technique further worsen these conditions. Many athletes ignore early symptoms, which can lead to chronic instability and long-term pain. Early evaluation by a sports injury specialist helps prevent complications and ensures a safe return to activity. Pain in Left Hand and Shoulder Pain that starts in the shoulder often radiates downward, causing discomfort in the arm and hand. This type of pain is commonly associated with nerve involvement or muscular tension extending from the shoulder joint. Possible reasons include: Nerve compression from shoulder inflammation Rotator cuff injuries affect arm movement Referred pain from cervical spine issues Pain in the arm combined with left shoulder pain should not be ignored, especially if accompanied by weakness or tingling sensations. Proper diagnosis helps distinguish between muscular strain and nerve-related conditions, ensuring targeted treatment and faster recovery. Left Side Back Shoulder Pain Left side back shoulder pain often originates from the muscles supporting the shoulder blade and upper spine. Poor posture, muscle imbalance, and overtraining are frequent contributors, particularly in athletes. Common factors include: Upper back muscle strain Scapular instability Improper training posture Weak core and back muscles This type of pain can restrict shoulder movement and reduce athletic performance. Strengthening the surrounding muscles and improving posture are essential for long-term relief and injury prevention. Symptoms of Left Shoulder Pain Symptoms of left shoulder pain vary depending on the underlying cause and severity of the condition. Some individuals experience sharp pain, while others notice a dull ache that worsens with activity. Common symptoms include: Pain during lifting or reaching movements Shoulder stiffness and limited mobility Weakness or instability in the joint Pain spreading to the arm or upper back Persistent symptoms may indicate structural damage within the joint. Advanced diagnostic methods and treatments, including the shoulder arthroscopy procedure and recovery, are often used to evaluate internal shoulder injuries accurately. Shoulder Pain Treatment Options Treatment for left shoulder pain depends on the severity of the condition and the patient’s activity level. Early-stage pain often responds well to conservative care, while severe injuries may require advanced medical intervention. Treatment options include: Rest and activity modification Anti-inflammatory medications Physiotherapy and rehabilitation exercises Sports injury medical management For cases involving internal joint damage, minimally invasive surgical procedures may be recommended. Timely treatment helps restore mobility, reduce pain, and prevent long-term complications. Left Shoulder Pain Exercises Exercises play a crucial role in managing and preventing left shoulder pain. Properly guided exercises improve strength, flexibility, and joint stability without increasing injury risk. Recommended exercises include: Gentle stretching for improved flexibility Strengthening exercises for rotator cuff muscles Posture-correcting movements Stability exercises for shoulder support Exercises should always be performed under professional guidance, especially after injury. Incorrect technique can worsen pain and delay recovery. When to See a Doctor Medical attention is necessary when left shoulder pain becomes persistent or interferes with daily activities. Ignoring symptoms can lead to chronic joint damage. Consult a doctor if: Pain lasts more than a few days Shoulder pain follows a sports injury or a fall There is difficulty lifting or moving the arm Numbness or weakness is present Early evaluation ensures accurate diagnosis and effective treatment planning. Key Takeaways for Managing Left Shoulder Pain Aspect Why It Matters Long-Term Benefit Early Diagnosis Identifies the root cause accurately Prevents chronic damage Proper Treatment Targets pain and inflammation Faster recovery Physiotherapy Restores strength and mobility Reduces re-injury risk Lifestyle Changes Corrects posture
Shoulder Arthroscopy for Sports Injuries and Chronic Shoulder Problems
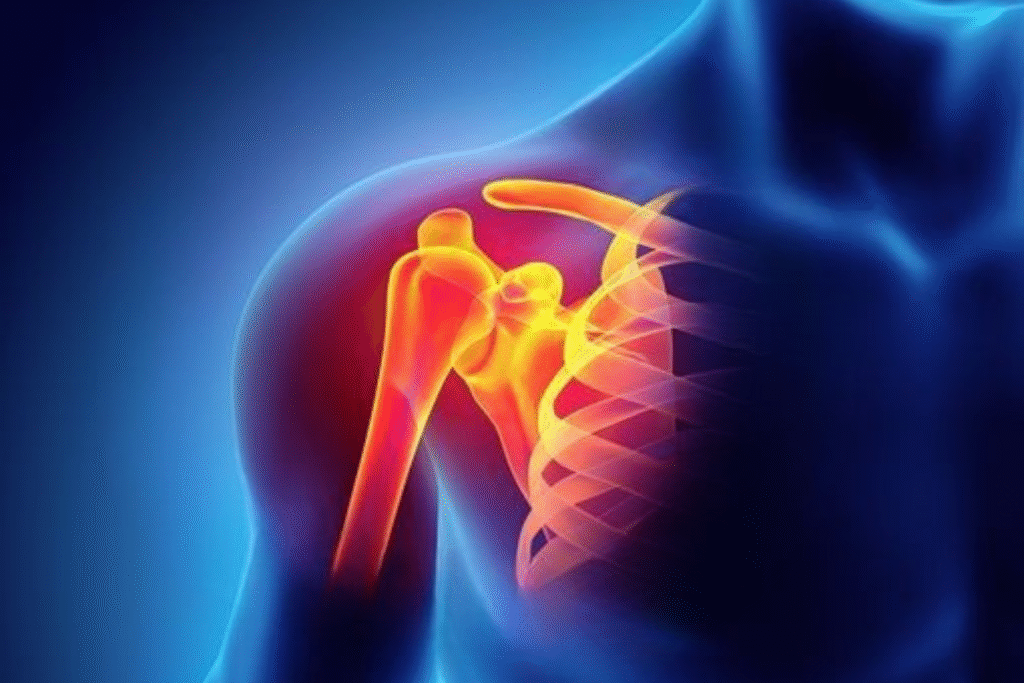
Shoulder Arthroscopy for Sports Injuries and Chronic Shoulder Problems Shoulder arthroscopy is a modern, minimally invasive surgical technique used to diagnose and treat various shoulder conditions. It is especially effective for sports injuries and long-standing shoulder problems that do not improve with medication or physiotherapy. Using a small camera and specialized instruments, surgeons can repair damaged tissues with precision, less pain, and faster recovery. This advanced procedure has become the preferred option for athletes and active individuals who want to return to normal activity safely and quickly. What Is Shoulder Arthroscopy? Shoulder arthroscopy is a surgical procedure in which a thin camera (arthroscope) is inserted into the shoulder joint through small incisions. The camera projects images onto a screen, allowing the surgeon to clearly view and treat internal joint problems. Conditions Treated with Shoulder Arthroscopy Rotator cuff tears Labral tears (SLAP lesions) Shoulder instability and dislocations Frozen shoulder Shoulder impingement syndrome Sports-related ligament and tendon injuries This technique reduces tissue damage and improves surgical accuracy compared to open surgery. Shoulder Arthroscopy for Sports Injuries Sports activities place repetitive stress on the shoulder joint. Over time or due to sudden trauma, this can result in pain and restricted movement. Shoulder arthroscopy is widely used to manage sports injuries effectively. Common Sports Injuries Requiring Shoulder Arthroscopy Rotator cuff injuries in cricket, tennis, and swimming Shoulder dislocations in contact sports Labral tears in throwing athletes Overuse injuries in weightlifters Benefits for Athletes Smaller incisions and minimal scarring – Shoulder arthroscopy uses tiny cuts, resulting in less tissue damage, minimal scarring, and better cosmetic outcomes. Faster healing and early rehabilitation – Minimal invasion allows quicker tissue healing, enabling patients to start physiotherapy and movement earlier. Improved joint stability – Precise repair of damaged ligaments and tendons helps restore shoulder strength and long-term joint stability. Quick return to sports activities – Athletes recover faster with structured rehab, allowing a safe and confident return to sports and training. Shoulder Arthroscopy for Chronic Shoulder Problems Chronic shoulder pain often develops due to untreated injuries, aging, or repetitive strain. When conservative treatments fail, shoulder arthroscopy becomes an effective long-term solution. Chronic Conditions Treated Long-standing rotator cuff degeneration Shoulder stiffness and frozen shoulder Chronic inflammation of the shoulder joint Persistent pain limiting daily activities Early surgical intervention helps prevent further joint damage and improves quality of life. Right Shoulder Arthroscopy – What You Should Know Right shoulder arthroscopy is commonly performed because the right shoulder is dominant for most individuals. The procedure and recovery process remain the same as for the left shoulder, but extra care is required post-surgery to manage daily tasks. Special Considerations Temporary work restrictions Modified driving habits Assistance with routine activities during early recovery Shoulder Arthroscopy Procedure – Step-by-Step Before Surgery Physical examination and imaging tests Pre-surgical fitness assessment Discussion of treatment goals During Surgery Small incisions around the shoulder Arthroscope insertion Repair of damaged tissues After Surgery Sling support for healing Pain management Start of guided physiotherapy The entire shoulder arthroscopy procedure usually lasts 1–2 hours. Shoulder Arthroscopy Recovery Timeline The shoulder arthroscopy recovery timeline depends on the type of injury, surgical repair, patient age, and rehabilitation, usually ranging from a few weeks to several months. Recovery Phases Week 1–2: Pain control and immobilization Week 3–6: Gentle movement and physiotherapy Week 6–12: Strengthening exercises 3–6 Months: Return to sports or heavy activity Following medical advice strictly ensures optimal healing. Shoulder Arthroscopy Exercises for Faster Recovery Proper rehabilitation after shoulder arthroscopy is essential to restore shoulder strength, flexibility, and stability. A structured physiotherapy program helps reduce stiffness, prevent complications, improve joint movement, and ensure safe, long-term recovery. Common Shoulder Arthroscopy Exercises Pendulum exercises – Gentle swinging motions that reduce stiffness, improve blood flow, and support early shoulder movement. Passive range-of-motion exercises – Assisted movements that improve flexibility without putting strain on the healing shoulder joint. Resistance band training – Light resistance exercises that gradually strengthen shoulder muscles and improve joint stability. Shoulder stabilization workouts – Controlled exercises that strengthen supporting muscles to enhance balance and prevent re-injury. These exercises should always be performed under a physiotherapist’s supervision to avoid complications. Shoulder Arthroscopy Cost – What to Expect The shoulder arthroscopy cost varies based on factors such as hospital facilities, surgeon’s experience, type of shoulder injury, diagnostic tests, anesthesia, hospital stay, and post-surgery rehabilitation, making each patient’s treatment cost different. Cost Influencing Factors Type of shoulder injury Diagnostic tests required Duration of hospital stay Rehabilitation and physiotherapy While the initial cost may seem higher, faster recovery and long-term relief make it a cost-effective solution. Advantages of Shoulder Arthroscopy Over Open Surgery Shoulder arthroscopy offers several advantages over open surgery due to its minimally invasive nature. It involves smaller incisions, which means less tissue damage, reduced pain, and minimal scarring. Patients usually experience a lower risk of infection, shorter hospital stays, and faster recovery. Early rehabilitation helps restore shoulder movement and strength, allowing patients to return to daily activities and sports more quickly and safely. Key Advantages Minimal blood loss Lower infection risk Less post-operative pain Faster recovery Shorter hospital stay These benefits make shoulder arthroscopy the preferred surgical approach worldwide. Who Is an Ideal Candidate for Shoulder Arthroscopy? You may be advised to undergo shoulder arthroscopy if: Pain persists despite medication and therapy – If shoulder pain continues even after medicines and physiotherapy, arthroscopy helps identify and treat the root cause. Shoulder movement is limited – When stiffness or reduced range of motion affects daily activities, shoulder arthroscopy can restore smooth joint movement. Sports performance is affected – Ongoing shoulder weakness or pain limiting sports activities may require arthroscopic repair for safe return to performance. Imaging shows structural damage – MRI or X-ray findings like tears or A proper orthopedic evaluation is essential before deciding on surgery. FAQs – Shoulder Arthroscopy Is shoulder arthroscopy a major surgery? No, it is a minimally invasive procedure with smaller incisions and quicker recovery compared to open surgery. How long does shoulder arthroscopy recovery take? Most patients
Knee Cartilage Health Guide: Injury Types, Pain & Recovery

Knee Cartilage Health Guide: Injury Types, Pain & Recovery Healthy knees play a vital role in maintaining mobility, independence, and overall quality of life. At the center of smooth knee movement lies Knee Cartilage, a specialized tissue that cushions the joint, absorbs shock, and prevents bones from rubbing against each other. When this cartilage is damaged or worn down, even simple activities such as walking, standing, or climbing stairs can become painful and restrictive. An in-depth overview of knee cartilage function, common injury types, pain symptoms, diagnostic methods, and modern recovery solutions, including Cartilage Repair & Regeneration, is designed to support informed decisions for long-term joint health and improved mobility. What Is Knee Cartilage and Why Is It Important? The arthroscopy meaning comes from two Greek words: arthro (joint) and skopein (to look). Arthroscopy refers to a medical technique that allows doctors to examine the inside of a joint using a small camera. Knee arthroscopy is a procedure in which a thin instrument called an arthroscope is inserted into the knee joint through tiny incisions. The camera attached to the arthroscope sends real-time images to a screen, enabling surgeons to closely inspect the knee’s internal structures, such as cartilage, ligaments, meniscus, and joint lining. Unlike traditional open surgery, knee arthroscopy causes minimal damage to surrounding tissues, making it a preferred option for both diagnosis and treatment. What Is Arthroscopic Knee Surgery and How Does It Work? Knee cartilage is a smooth, flexible connective tissue that covers the ends of bones within the knee joint. It allows frictionless movement while distributing body weight evenly across the joint. Unlike muscles or bones, cartilage has a very limited blood supply, which means healing is slow and often incomplete without medical support. There are two primary forms found in the knee: Articular cartilage, which covers the ends of the femur, tibia, and patella Meniscal cartilage, which acts as a shock absorber and stabilizer When knee cartilage damage occurs, joint mechanics are disrupted, leading to pain, inflammation, and progressive degeneration. Common Causes of Knee Cartilage Damage Cartilage injuries may occur suddenly or develop gradually over time. Common contributing factors include: Sports-related trauma or twisting injuries, often seen during sudden direction changes or high-impact activities Repetitive stress from physical work that places a continuous load on the knee joint Age-related degeneration, where cartilage naturally thins and loses elasticity Obesity and excess joint load increase pressure on the knee surfaces with every step Poor posture or joint alignment, causing uneven stress distribution When ignored, early damage can quietly worsen, eventually leading to loss of cartilage in the knee and a higher risk of osteoarthritis. Types of Knee Cartilage Injuries Understanding the nature of cartilage injuries helps guide appropriate treatment and recovery expectations. 1. Focal Cartilage Defects Small, localized areas of cartilage damage are usually caused by a sudden injury or direct impact Common in younger or active individuals after sports accidents Pain is often activity-related and may worsen with weight-bearing Early treatment can prevent the damage from spreading 2. Degenerative Cartilage Wear Develops gradually over time due to aging or long-standing joint stress Cartilage becomes thinner and less flexible, reducing shock absorption Symptoms often start as stiffness or mild pain and worsen slowly Frequently associated with osteoarthritis 3. Meniscus Tears Meniscus Tears occurs when the knee twists suddenly while bearing weight Often felt as sharp pain, locking, or catching in the joint Swelling may appear hours after injury rather than immediately Common in athletes as well as older adults with weakened cartilage 4. Full-Thickness Cartilage Loss Represents advanced damage where cartilage is completely worn away Causes bone-on-bone contact, leading to severe pain and stiffness Movement becomes difficult, and daily activities are affected Usually requires advanced medical or surgical intervention Knee Cartilage Damage Symptoms to Watch For Early recognition of knee cartilage damage symptoms is essential for preventing further deterioration. Common warning signs include: Persistent knee discomfort during movement Swelling or stiffness after activity Clicking, grinding, or locking sensations Reduced flexibility Instability while walking Many patients initially ignore mild knee cartilage pain, assuming it will resolve on its own. Unfortunately, delayed treatment often leads to worsening joint health. How Knee Cartilage Problems Are Diagnosed Accurate diagnosis is key to effective management, as early cartilage damage may cause symptoms even before clear changes appear on standard imaging. Careful evaluation helps identify the extent of injury, prevent progression, and support timely, joint-preserving treatment decisions. Specialists typically use: Clinical examination and movement assessment X-rays to assess joint space narrowing MRI scans to evaluate cartilage structure Arthroscopy for direct visualization Early diagnosis allows for more conservative and joint-preserving treatment options. Knee Cartilage Damage Treatment Options Treatment depends on injury severity, patient age, activity level, and overall joint condition. Knee cartilage damage treatment usually follows a stepwise approach. Non-Surgical Treatment Approaches For mild to moderate cases: Activity modification Physiotherapy and muscle strengthening Weight management Anti-inflammatory medications Joint injections Many patients explore knee cartilage repair without surgery to delay invasive procedures and maintain daily function. Can Knee Cartilage Regenerate? A common question is: Can knee cartilage regenerate naturally?Due to limited blood supply, the natural healing capacity is poor. However, advances in medical science now support knee cartilage regeneration using biological techniques that stimulate repair or replace damaged tissue. Surgical Options for Cartilage Repair When conservative methods fail, surgical intervention may be required. Modern knee cartilage surgery focuses on joint preservation rather than replacement. Common Procedures Include: Microfracture surgery Autologous chondrocyte implantation Osteochondral grafting Advanced cartilage reconstruction techniques These procedures aim to restore cushioning and delay joint replacement. Knee Cartilage Repair Techniques Explained Different approaches are used depending on defect size and location. Knee cartilage repair procedures are designed to improve mobility, reduce pain, and restore joint stability. Treatment Option Best For Invasiveness Expected Recovery Physiotherapy Mild damage Non-invasive 4–8 weeks Injections Pain control Minimally invasive Few days Microfracture Small defects Surgical 3–6 months Cartilage grafting Moderate damage Surgical 6–12 months Advanced repair techniques Severe damage Surgical 9–12 months This table helps patients understand
Understanding Arthroscopic Knee Surgery: When It’s Needed & Benefits
Understanding Arthroscopic Knee Surgery: When It’s Needed & Benefits Knee pain and restricted movement can significantly affect daily life, work performance, and physical activity. For individuals dealing with persistent knee problems that do not improve with medication or physiotherapy alone, advanced medical procedures may become necessary. One such widely used and effective procedure is arthroscopic knee surgery, a minimally invasive technique that allows accurate diagnosis and treatment of various knee joint conditions.This approach has transformed knee care by reducing surgical trauma, improving recovery time, and offering better outcomes for both active individuals and older patients. Understanding how the procedure works, when it is required, and what results to expect can help patients make informed decisions about their knee health. Arthroscopy Meaning and What Is Knee Arthroscopy The arthroscopy meaning comes from two Greek words: arthro (joint) and skopein (to look). Arthroscopy refers to a medical technique that allows doctors to examine the inside of a joint using a small camera. Knee arthroscopy is a procedure in which a thin instrument called an arthroscope is inserted into the knee joint through tiny incisions. The camera attached to the arthroscope sends real-time images to a screen, enabling surgeons to closely inspect the knee’s internal structures, such as cartilage, ligaments, meniscus, and joint lining. Unlike traditional open surgery, knee arthroscopy causes minimal damage to surrounding tissues, making it a preferred option for both diagnosis and treatment. What Is Arthroscopic Knee Surgery and How Does It Work? Arthroscopic knee surgery is a surgical procedure performed using arthroscopy to treat identified knee problems. After the knee is examined, specialized instruments are inserted through small incisions to repair or remove damaged tissue. This procedure is commonly used to: Repair a torn meniscus Treat ligament injuries Smooth damaged cartilage Remove loose bone or cartilage fragments. Address inflammation within the knee joint. Because it is minimally invasive, arthroscopic knee surgery results in less pain, reduced scarring, and faster recovery compared to open knee surgery. Diagnostic Arthroscopy Knee: When Imaging Is Not Enough In some cases, MRI or X-ray scans may not clearly explain ongoing knee pain. Diagnostic arthroscopy knee plays an important role in such situations. This procedure allows direct visualization of the knee joint, helping specialists identify: Hidden cartilage damage Small ligament tears Early joint degeneration Inflammatory conditions Diagnostic arthroscopy knee is especially useful when symptoms persist despite normal imaging results, ensuring accurate diagnosis and appropriate treatment planning. Conditions Treated Using Knee Arthroscopy Knee arthroscopy is commonly used to treat a wide range of knee problems, including: Meniscus tears ACL and PCL ligament injuries Cartilage wear and degeneration Synovial inflammation Loose bodies within the joint Sports-related knee injuries Due to its precision, arthroscopic knee surgery is often recommended for athletes, physically active individuals, and patients experiencing mechanical knee symptoms such as locking or catching. How Successful Is Arthroscopic Knee Surgery A common concern among patients is how successful arthroscopic knee surgery is. Success largely depends on the type of knee condition, overall joint health, and adherence to rehabilitation protocols. In general: Meniscus repairs and ligament treatments show high success rates Sports injuries respond well to proper physiotherapy. Younger and active patients often recover faster. Early intervention improves long-term joint function. When performed for the right indication, arthroscopic knee surgery provides excellent symptom relief and functional improvement. Arthroscopic Knee Surgery Cost Arthroscopic knee surgery cost may vary based on procedure purpose, hospital infrastructure, surgeon experience, and whether knee arthroscopy is used for diagnosis or treatment. Factors influencing cost include: Hospital infrastructure Surgeon’s expertise Type of anesthesia used Complexity of the knee condition Duration of hospital stay In many cases, insurance policies cover knee arthroscopy when medically indicated. Patients are advised to discuss cost details and coverage options beforehand. Knee Arthroscopy Recovery Time and Healing Process One of the biggest advantages of arthroscopic procedures is a shorter knee arthroscopy recovery time. Most patients can walk on the same day or within a few days after surgery. Typical recovery timeline: Mild pain and swelling for a few days Return to desk work within 1–2 weeks. Physiotherapy starts early to restore strength. Full recovery may take 4–8 weeks, depending on the procedure. Proper rehabilitation plays a crucial role in ensuring long-term success and preventing stiffness or weakness. Comparison Table: Arthroscopic Surgery vs Open Knee Surgery Feature Arthroscopic Knee Surgery Open Knee Surgery Incision size Very small Large incision Pain after surgery Mild to moderate Moderate to severe Recovery time Faster Longer Infection risk Lower Higher Hospital stay Short or same day Longer Scarring Minimal Visible scars This comparison highlights why knee arthroscopy has become the preferred choice for many knee conditions. Benefits of Arthroscopic Knee Surgery The growing popularity of arthroscopic knee surgery is due to its multiple benefits, especially its ability to address knee problems with precision while minimizing tissue damage and supporting quicker functional recovery for patients. Minimally invasive approach Reduced postoperative pain Faster recovery and rehabilitation Lower complication rates Better preservation of knee joint structures Quicker return to daily activities and sports These advantages make it an effective solution for both diagnostic and therapeutic purposes. Risks and Limitations of Knee Arthroscopy While generally safe, knee arthroscopy is still a surgical procedure and carries some risks, including temporary discomfort related to healing, individual response to anesthesia, and variations in recovery depending on overall joint health and activity level, including: Temporary swelling or stiffness Infection (rare) Blood clots (very uncommon) Incomplete symptom relief if arthritis is advanced It may not be suitable for severe joint degeneration, where joint replacement becomes a better option. Who Should Consider Arthroscopic Knee Surgery Arthroscopic knee surgery may be recommended for individuals who: Have persistent knee pain despite conservative treatment Experience locking or instability Suffer from sports-related knee injuries Need a precise diagnosis of unexplained knee symptoms. A thorough evaluation by a knee specialist helps determine whether knee arthroscopy is appropriate. Role of Rehabilitation and Physiotherapy Physiotherapy is essential after
What Is a Knee Ligament Injury? Symptoms, Treatment & Recovery

What Is a Knee Ligament Injury? Symptoms, Treatment & Recovery The knee is one of the most active and important joints in the human body. It supports body weight, allows movement, and absorbs shock during daily activities such as walking, climbing stairs, running, or playing sports. Because of this constant use, the knee can easily get injured, particularly the ligaments. A knee ligament injury can suddenly limit mobility and make even simple movements uncomfortable or painful. For many people, a knee injury brings uncertainty. Questions about recovery time, treatment options, and long-term impact are common. With the right understanding, timely medical care, and a structured rehabilitation plan, most individuals can recover well and regain confidence in knee movement. This guide explains the condition in a clear, human, and practical manner. Understanding Knee Ligament Injury Ligaments are strong yet flexible connective tissues that join bones together and guide joint motion. In the knee, ligaments work together to maintain stability while allowing controlled movement. When one of these ligaments is overstretched or torn, joint balance is affected, leading to pain, swelling, and instability. Major Ligaments of the Knee Anterior Cruciate Ligament (ACL): Controls forward movement and rotational stability Posterior Cruciate Ligament (PCL): Prevents backward movement of the shinbone Medial Collateral Ligament (MCL): Supports the inner side of the knee Lateral Collateral Ligament (LCL): Stabilizes the outer side of the knee Damage to any of these structures may result in a knee ligament injury that ranges from mild stretching to complete rupture. Common Causes of Knee Ligament Injury Knee ligament damage usually occurs when the joint is forced into an unnatural position. Sudden movements or external force are the most common triggers. Frequent Causes Include Sudden twisting or pivoting of the knee Landing awkwardly after jumping Direct impact during sports or accidents Slipping or falling on uneven surfaces Road traffic accidents While athletes are at higher risk due to intense physical activity, non-athletes can also experience knee ligament injury during routine daily movements. Knee Ligament Injury Symptoms Recognizing knee ligament injury symptoms early plays an important role in preventing further damage and improving recovery outcomes. Early Symptoms Sudden pain at the time of injury Swelling develops within a few hours Stiffness or reduced range of motion Tenderness around the knee joint Progressive Symptoms Knee instability or a feeling of giving way Difficulty bearing weight on the affected leg Pain while walking or climbing stairs Reduced confidence during movement Ignoring these signs may prolong the knee ligament injury recovery period and increase the risk of chronic joint problems. Diagnosis of Knee Ligament Injury Proper diagnosis helps determine the severity of injury and the most effective treatment plan. Clinical Examination A specialist evaluates: Knee stability Pain response Range of motion Ligament integrity through physical tests Imaging Tests X-rays: Used to rule out fractures or bone injury MRI scans: Provide detailed images of ligament tears and soft tissue damage Accurate diagnosis supports better treatment decisions and helps shorten knee ligament injury recovery time. Knee Ligament Injury Treatment Options Treatment is tailored according to the severity of injury, activity level, and individual needs. Non-Surgical Knee Ligament Injury Treatment Many ligament injuries heal well without surgery when managed correctly. Conservative care may include: Rest and temporary activity modification Ice application to reduce swelling Anti-inflammatory medications Structured physiotherapy programs This approach is commonly recommended for mild to moderate injuries with stable knee joints. Surgical Treatment Surgery may be advised when: A ligament is completely torn Knee instability persists despite rehabilitation High joint performance is required for sports or work Post-surgical rehabilitation is essential for restoring knee strength and function. Knee Ligament Injury Treatment Exercises Exercise-based rehabilitation is a key part of healing and long-term knee stability. Early-Phase Exercises Gentle range-of-motion movements Isometric quadriceps contractions Straight leg raises Strengthening and Control Phase Hamstring and quadriceps strengthening Balance and coordination training Controlled functional movements Knee ligament injury treatment exercises should always be performed under professional supervision to avoid complications. Knee Support for Ligament Injury External knee support can provide extra stability during recovery, and using a knee brace for ACL injuries helps protect the joint, reduce strain on healing ligaments, and improve confidence in movement. Benefits of Knee Support Reduces stress on healing ligaments Improves joint alignment Enhances confidence during walking Minimizes sudden knee instability Common Types of Support Elastic compression sleeves Hinged knee braces Functional sports braces The choice of knee support for ligament injury depends on the stage of recovery and activity level. Knee Ligament Injury Recovery Period The knee ligament injury recovery period varies from person to person and depends on multiple factors. Factors Affecting Recovery Type of ligament involved Grade of injury Treatment approach Age and overall physical condition Estimated Recovery Period Injury Grade Treatment Method Expected Recovery Period Grade 1 (Mild) Rest and physiotherapy 2–4 weeks Grade 2 (Moderate) Brace and rehab 6–10 weeks Grade 3 (Severe) Surgery and rehab 6–9 months Consistency and patience are essential throughout recovery. Knee Ligament Injury Recovery Time and Healing Stages The knee ligament injury recovery time follows a structured biological healing process. Healing Stages Inflammation: Pain and swelling management Repair: Tissue regeneration and strengthening Remodeling: Restoration of function and stability Returning to high-impact activities too early can delay healing and increase re-injury risk. Nutrition and Supportive Care Rehabilitation outcomes improve when supported by proper nutrition, healthy lifestyle habits, and consistent adherence to physiotherapy exercises. Proper nutrition helps strengthen the body, reduces inflammation, and promotes faster overall healing. Knee Ligament Injury Recovery Food Protein-rich foods to support tissue repair Vitamin C for collagen production Calcium and vitamin D for joint strength Adequate hydration for flexibility and circulation Balanced nutrition supports healing, boosts energy levels, and aids recovery, but it does not replace professional medical treatment and rehabilitation guidance. Recovery Timeline Based on Treatment Approach Treatment Type Walking Comfort Daily Activities Sports Readiness Conservative care 2–3 weeks 4–6 weeks 8–12 weeks Surgical treatment 4–6 weeks 3–4 months 6–9 months This timeline helps patients set realistic expectations during recovery. Daily Life
How to Prevent Hamstring Injury in Athletes: Warm-ups & Mobility

How to Prevent Hamstring Injury in Athletes: Warm-ups & Mobility Hamstring injuries are one of the most common challenges athletes face across sports that involve sprinting, jumping, kicking, and rapid directional changes. Whether it’s football, athletics, tennis, cricket, or basketball, the hamstring muscles are constantly under pressure. When they become overloaded, fatigued, or poorly conditioned, the chances of injury rise sharply, highlighting the importance of proper Muscle Strain & Hamstring Treatment for effective recovery and long-term injury prevention. Learning how to prevent hamstring injury in athletes is essential not only for safety but also for sustaining long-term performance. A well-prepared hamstring is stronger, more flexible, and less likely to tear. This blog explains the best warm-ups, the most effective mobility drills, and the real reasons hamstrings get injured — helping athletes stay active, confident, and injury-free. Why the Hamstrings Get Injured So Often The hamstrings include three muscles at the back of the thigh—biceps femoris, semitendinosus, and semimembranosus. These muscles work together to bend the knee, extend the hip, and support fast, explosive actions. Hamstring injuries happen due to: Sudden acceleration or sprinting Poor warm-up or inadequate muscle preparation Weak glutes or muscle imbalances Tight hip flexors leading to overcompensation Fatigue during late-game movements Previous hamstring injury Poor running mechanics Athletes who understand these factors are easier to coach and more aware of their body limits. This awareness already reduces the risk of injury dramatically. Warm-Up Routines That Dramatically Reduce Hamstring Injury Risk A proper warm-up is the foundation of injury prevention. It prepares the nervous system, increases blood flow, boosts flexibility, and enhances muscle elasticity. Warm-ups should be dynamic, controlled, and sport-specific. Below are the most effective warm-up drills. Each one plays a unique role in strengthening or activating the hamstring muscles. 1. Dynamic Leg Swings Dynamic leg swings are highly effective in loosening tight hamstrings and improving hip mobility. The movement prepares the leg for natural forward motion, similar to running mechanics. Why this helps: Enhances stride length Improves hip extension Activates the hamstring without overstretching This is often used by athletes before sprinting sessions or explosive sports activities. 2. High Knees High knees increase your heart rate while activating the hip flexors, glutes, and hamstrings. They also improve coordination and running posture. Benefits include: Better blood flow Improved muscle readiness Reduced stiffness in lower-body muscles Just 30–45 seconds of high knees can prepare the body for faster-paced warm-ups. 3. Walking Lunges Walking lunges strengthen the entire lower body, particularly the glutes, which play a critical role in preventing hamstring injury. Lunges also stretch the hip flexors, which reduces tension on the hamstrings. This movement is essential for athletes whose sports demand agility, balance, and direction changes. 4. Butt Kicks and A-Skips These drills mimic sports movements and prepare the legs for acceleration. They help athletes naturally engage the hamstrings without causing strain. Why athletes use them: Improve running mechanics Activate lower-body muscles Boost neuromuscular coordination Even elite sprinters and footballers regularly perform these drills to reduce injury risks. Mobility Routines Athletes Should Not Skip Warm-ups help activate the muscles, but mobility work improves flexibility and range of motion. Without proper mobility, the hamstrings become tight and more vulnerable to strain. These routines significantly reduce the chances of injury: 1. Active Hamstring Stretch Active stretching involves controlled leg lifting while keeping the movement fluid. This improves flexibility without reducing muscle power. Athletes prefer active stretching over static holds before training. What it improves: Muscle elasticity Balance in the lower body Ability to move comfortably through full range This is especially important for preventing overstretch injuries during sprinting. 2. Hip Flexor Mobility When hip flexors become tight (which is very common in athletes who sit a lot), the pelvis tilts forward. This puts additional strain on the hamstrings. Benefits of hip-flexor mobility: Better pelvic alignment Reduced hamstring overload Improved posture and stride Many hamstring issues are actually a result of hip tightness—not hamstring weakness. 3. Glute Activation A weak glute forces the hamstrings to overcompensate, especially during acceleration. Activating and strengthening the glutes helps redistribute the workload correctly. Recommended activation options: Mini-band lateral walks Clamshells Glute bridges These exercises strengthen surrounding muscles and help protect the hamstrings from unnecessary stress. 4. Eccentric Strengthening (Nordic Curls) Nordic hamstring curls are one of the most researched and proven exercises for preventing hamstring strains. They train the muscle to remain strong even when it is lengthening — the exact moment when strains occur. This significantly lowers injury risk and improves hamstring resilience. Weekly Prevention Routine for Athletes Maintaining a balanced weekly routine helps athletes keep their hamstrings strong, flexible, and less prone to strain. By combining warm-ups, strength work, mobility, and recovery, the muscles stay conditioned throughout training and minimize injury risks. Here’s a simple weekly routine athletes can follow to prevent hamstring strain: 2 days of dynamic lower-body warm-ups 2 days of eccentric strength training (Nordic curls) Daily light mobility stretching 1 day dedicated to soft-tissue work and recovery This combination supports flexibility, strength, and overall healthy muscle function. If a Strain Happens: What Athletes Should Do First Even with proper care, minor strains can still happen. Faster recovery depends on immediate action. First Steps: Reduce physical load Apply ice to control swelling Avoid deep stretching in the first 48 hours Begin light mobility only when pain decreases Progress towards hamstring strain exercises slowly Following the correct recovery protocol reduces the overall hamstring strain recovery time and prevents re-injury. Once improving, athletes can explore internal guidance such as muscle strain of hamstring treatment. Long-Term Strategies to Prevent Hamstring Injury Consistency is more important than intensity. Athletes who incorporate small but meaningful habits into their training see the best results. Long-term prevention habits include: Warm-ups before every session Regular hip and hamstring mobility Glute strengthening twice weekly Improving stride mechanics Maintaining hydration Resting between heavy workouts Listening to muscle tightness and early signs







