Knee Cap for Pain Relief: Benefits, Types, and How It Supports Knee Recovery

Knee Cap for Pain Relief: Benefits, Types, and How It Supports Knee Recovery Knee pain is a common problem that affects people of all ages. Whether it is caused by injury, arthritis, overuse, or muscle weakness, knee pain can significantly affect daily activities such as walking, climbing stairs, and exercising. One of the most commonly recommended support tools for managing knee discomfort is a knee cap for pain relief. A knee cap for pain relief helps stabilise the knee joint, reduce pressure on the muscles and ligaments, and provide compression that can decrease swelling and discomfort. Many doctors and physiotherapists recommend using a knee cap along with proper knee pain treatment, exercises, and lifestyle modifications for better recovery. In this blog, we will explore how a knee cap for pain relief works, its benefits, different types available, and how it supports long-term knee recovery. What Is a Knee Cap for Pain Relief? A knee cap for pain relief is a supportive orthopaedic brace designed to provide compression, stability, and protection to the knee joint. It is commonly made of elastic, neoprene, or fabric materials that fit snugly around the knee. People suffering from knee joint pain, sports injuries, ligament strain, arthritis, or muscle weakness often use a knee cap for pain relief to reduce stress on the knee and improve mobility. Doctors often include a knee cap for pain relief as part of a comprehensive knee pain treatment plan because it helps protect the joint during daily movement and physical activity. Common Knee Pain Causes Understanding the knee pain causes can help determine when a knee cap for pain relief may be beneficial. Knee pain can develop due to several reasons, including: 1. Ligament Injuries Injuries such as ACL or MCL tears can cause instability and pain in the knee joint. 2. Arthritis Osteoarthritis is one of the most common knee pain causes, especially in older adults. It occurs when the cartilage in the knee joint gradually wears down. 3. Meniscus Tear The meniscus is a cartilage that cushions the knee joint. A tear can cause severe knee joint pain and swelling. 4. Overuse or Sports Injuries Athletes and physically active individuals often experience knee pain due to repetitive stress on the joint. 5. Muscle Weakness Weak muscles around the knee can increase stress on the joint, leading to chronic discomfort. Using a knee cap for pain relief in such conditions can help stabilize the joint and reduce pressure on injured tissues. Benefits of Using a Knee Cap for Pain Relief A knee cap for pain relief provides several advantages for people suffering from knee discomfort. Here are some of the key benefits: 1. Provides Joint Stability One of the main benefits of a knee cap for pain relief is that it stabilises the knee joint. It helps prevent abnormal movements that may worsen injuries. 2. Reduces Swelling and Inflammation Compression from a knee cap for pain relief improves blood circulation around the knee and helps reduce swelling. 3. Supports Knee Recovery During rehabilitation, wearing a knee cap for pain relief can support healing tissues and protect the knee from further damage. 4. Improves Mobility People suffering from knee joint pain often find it difficult to walk or perform physical activities. A knee cap for pain relief can make movement easier and more comfortable. 5. Prevents Further Injury For athletes or individuals recovering from injury, a knee cap for pain relief provides extra support that reduces the risk of further knee damage. Types of Knee Cap for Pain Relief There are different types of knee cap for pain relief available depending on the severity of knee pain and the level of support needed. 1. Compression Knee Cap This type of knee cap for pain relief provides gentle compression to improve circulation and reduce swelling. It is commonly used for mild knee joint pain. 2. Patellar Support Knee Cap This knee brace has a special opening around the kneecap to support the patella and reduce pressure. 3. Hinged Knee Cap A hinged knee cap for pain relief provides strong support and is often recommended after ligament injuries or surgery. 4. Elastic Knee Cap Elastic knee caps are lightweight and flexible. They are ideal for daily use and mild knee pain treatment. Choosing the right knee cap for pain relief depends on the cause and severity of the knee problem. How a Knee Cap Supports Knee Recovery A knee cap for pain relief plays an important role in the recovery process by supporting the knee joint and surrounding muscles. 1. Reduces Pressure on the Knee Joint By providing compression and support, a knee cap for pain relief reduces the load on the knee joint. 2. Improves Blood Circulation Better circulation helps deliver oxygen and nutrients to injured tissues, promoting faster healing. 3. Helps Maintain Proper Alignment Proper knee alignment reduces strain on ligaments and cartilage, which is essential for recovery. 4. Encourages Safe Movement When people experience knee joint pain, they often avoid movement. A knee cap for pain relief gives confidence and support for safe movement. Knee Pain Exercises for Knee Pain Along with using a knee cap for pain relief, performing proper knee pain exercises for knee pain can strengthen the muscles around the knee and reduce pain. 1. Straight Leg Raises This exercise strengthens the quadriceps muscles without putting pressure on the knee joint. 2. Hamstring Stretch Stretching the hamstring muscles improves flexibility and reduces knee strain. 3. Heel Slides Heel slides help improve knee mobility and reduce stiffness. 4. Quadriceps Strengthening Strong quadriceps muscles provide better support to the knee joint and help in knee pain treatment. Regular knee pain exercises for knee pain combined with a knee cap for pain relief can significantly improve knee stability and recovery. When Should You Use a Knee Cap for Pain Relief? A knee cap for pain relief is commonly recommended in the following situations: Mild to moderate knee joint pain Sports injuries Ligament strain or instability Arthritis-related knee
Knee Ligament Tear Symptoms: Early Signs, Causes & Treatment Options

Knee Ligament Tear Symptoms: Early Signs, Causes & Treatment Options The knee joint plays a crucial role in everyday movement, such as walking, running, climbing stairs, and participating in sports. Because of its complex structure and constant use, the knee is vulnerable to injuries. One of the most common and serious injuries affecting the knee is a knee ligament tear. Recognising knee ligament tear symptoms early is extremely important because untreated ligament injuries can lead to long-term knee instability, chronic pain, and difficulty performing daily activities. The knee contains several strong tissues called knee ligaments that connect bones together and keep the knee joint stable. When these ligaments become overstretched or torn, it results in a knee ligament injury that may require medical treatment, physiotherapy, or even knee ligament surgery in severe cases. In this comprehensive guide, we will explore the knee ligament tear symptoms, causes, diagnosis, and the best knee ligament injury treatment options available. Understanding Knee Ligaments and Their Function Before learning about knee ligament tear symptoms, it is important to understand how the knee works. The knee is supported by several knee joint ligaments that stabilise the joint and allow smooth movement. These ligaments hold the bones together and prevent excessive movement that could damage the joint. The four main ligaments of the knee include: Anterior Cruciate Ligament (ACL) The ACL is one of the most important knee ligaments. It controls the forward movement of the shin bone and prevents the knee from rotating excessively. Posterior Cruciate Ligament (PCL) The PCL stabilizes the knee by preventing the shin bone from moving backward. Medial Collateral Ligament (MCL) The MCL supports the inner side of the knee and protects it from inward bending forces. Lateral Collateral Ligament (LCL) The LCL supports the outer side of the knee and helps maintain stability during movement. In addition to these major ligaments, the coronary ligament knee structures help anchor the meniscus and maintain joint stability. When any of these structures become damaged, it leads to a knee ligament injury that may affect mobility and joint function. Knee Ligament Tear Symptoms Identifying knee ligament tear symptoms early can help prevent complications and ensure timely treatment. The symptoms may vary depending on which ligament is injured and how severe the damage is. Sudden Knee Pain One of the earliest knee ligament tear symptoms is sudden and intense pain in the knee joint. The pain usually occurs immediately after the injury and may worsen when attempting to move or place weight on the knee. Swelling Around the Knee Swelling is another common sign of a knee ligament injury. The knee may swell within a few hours due to inflammation or internal bleeding within the joint. Swelling often causes tightness and discomfort around the knee. Knee Instability A feeling of instability is one of the most noticeable knee ligament tear symptoms. Many patients describe the sensation that the knee might “give out” while walking or standing. This occurs because damaged knee joint ligaments are no longer able to stabilize the joint properly. Difficulty Walking A knee ligament tear can make walking painful and difficult. Some people may limp or avoid putting weight on the injured leg. Severe injuries may prevent the person from walking at all. Limited Range of Motion Another sign of knee ligament tear symptoms is stiffness or restricted movement. The knee may not fully bend or straighten due to swelling and ligament damage. Popping Sound at the Time of Injury Many individuals report hearing a popping sound at the moment the injury occurs. This popping sensation is commonly associated with serious knee ligament injuries, particularly ACL tears. Causes of Knee Ligament Tear Several factors can cause a knee ligament injury. These injuries frequently occur during sports activities or sudden movements. Common causes include: Sports Activities Sports that involve jumping, running, or sudden direction changes can place stress on the knee ligaments and cause injuries. Sudden Twisting Movements Twisting the knee while the foot remains planted on the ground can damage the knee joint ligaments. Direct Impact to the Knee A strong blow to the knee during sports or accidents can lead to a knee ligament tear. Improper Landing Landing incorrectly after a jump can put excessive pressure on the knee ligaments. Risk Factors for Knee Ligament Injuries Certain factors increase the likelihood of developing knee ligament tear symptoms. These include: Participation in high-impact sports Weak thigh or hamstring muscles Poor exercise techniques Inadequate warm-up before physical activity Previous knee injuries Athletes involved in football, basketball, and skiing are particularly vulnerable to knee ligament injury. Diagnosis of Knee Ligament Injury When a patient experiences knee ligament tear symptoms, a proper medical evaluation is necessary. Doctors typically perform: Physical Examination The doctor examines the knee for swelling, tenderness, and instability. Imaging Tests Medical imaging helps confirm the diagnosis and determine the severity of the injury. Common imaging tests include: X-rays MRI scans Ultrasound MRI scans are particularly effective for examining knee ligaments and identifying ligament tears. Knee Ligament Injury Treatment Options Treatment depends on the severity of the injury and the patient’s lifestyle. Non-Surgical Treatment Many mild injuries can be treated without surgery. 1.Rest and Ice – Resting the knee and applying ice packs can reduce swelling and pain. 2.Knee Braces – Braces support the knee joint and help stabilize damaged knee joint ligaments during recovery. 3.Physiotherapy – Physical therapy is an essential part of knee ligament injury treatment. It strengthens the muscles around the knee and improves joint stability. Surgical Treatment Severe injuries may require knee ligament surgery. Surgical procedures are performed to repair or reconstruct the damaged ligament using graft tissue. Modern knee ligament surgery techniques often use arthroscopy, a minimally invasive method that allows faster recovery and less scarring. Recovery After Knee Ligament Surgery Recovery from knee ligament surgery typically occurs in stages. Initial Healing Phase Swelling and pain are managed while gentle movement begins. Rehabilitation Phase Physiotherapy helps restore strength and flexibility. Return to Activity Patients gradually return to normal
Shoulder Immobilizer: Types, Uses, Benefits & When Doctors Recommend It

Shoulder Immobilizer: Types, Uses, Benefits & When Doctors Recommend It Shoulder injuries can significantly restrict arm movement and affect daily activities. A shoulder immobilizer is specifically designed to stabilize the shoulder joint, reduce excessive motion, and support healing after injury, surgery, or shoulder instability. People searching for a shoulder immobilizer often want to know how it differs from a sling, whether it helps manage left shoulder pain causes, and when doctors actually recommend using one for recovery. Unlike a basic arm sling that mainly supports the forearm, a shoulder immobilizer keeps the arm firmly secured against the body to prevent rotation and sudden movement. This guide explains the types of shoulder immobilizers, their uses and benefits, and when doctors recommend a shoulder immobilizer for safe healing and long-term shoulder stability. What Is a Shoulder Immobilizer? A shoulder immobilizer is a structured orthopedic support brace designed to keep the arm securely positioned against the body, restrict shoulder movement, reduce joint strain, and promote proper healing after injury or surgery. Shoulder immobilizers are commonly recommended for people experiencing: • Shoulder dislocation• Rotator cuff injury• Shoulder instability• Post-surgical recovery• Severe left shoulder pain By stabilizing the joint and limiting unnecessary motion, a shoulder immobilizer protects injured ligaments, tendons, and muscles during the early healing phase. Types of Shoulder Immobilizers Different types of shoulder immobilizers are available depending on the severity of injury and the level of support required. Choosing the right type depends on medical advice and recovery needs. 1. Standard Shoulder Immobilizer A standard shoulder immobilizer includes an arm pouch and supportive straps that wrap aroundthe torso. • Provides firm joint stabilization• Limits shoulder rotation• Supports surgical recovery• Keeps arm secured to body 2. Shoulder Immobilizer Belt A shoulder immobilizer belt provides additional torso compression and enhanced restriction compared to a regular sling. • Offers stronger chest support• Prevents accidental arm movement• Enhances joint restriction• Helps manage shoulder instability 3. Universal Shoulder Immobilizer A universal shoulder immobilizer is adjustable and suitable for either shoulder. • Fits multiple body sizes• Easy to wear and remove• Suitable for mild injuries• Provides balanced positioning Selecting the correct shoulder immobilizer ensures effective stabilization and comfort during recovery. Common Left Shoulder Pain Causes Understanding left shoulder pain causes helps determine when immobilization is necessary and when rehabilitation may be more appropriate. Common left shoulder pain reasons include: • Rotator cuff tear• Frozen shoulder condition• Muscle strain injury• Shoulder instability episodes• Tendon inflammation In cases where movement increases pain or instability, doctors may recommend a shoulder immobilizer to reduce strain and allow proper tissue healing. Shoulder Immobilizer Uses The uses of a shoulder immobilizer extend beyond simple support. It plays an important role in protecting the joint and preventing further injury. Common shoulder immobilizer uses include: • Stabilizing the joint after dislocation• Supporting post-surgical healing• Preventing excessive shoulder rotation• Reducing swelling and inflammation• Protecting healing ligaments Doctors often prescribe a shoulder immobilizer before starting shoulder stretching exercises or strengthening programs. Benefits of a Shoulder Immobilizer Using a shoulder immobilizer correctly provides several therapeutic benefits during the acute injury phase. Key benefits include:• Reduces joint movement• Controls acute shoulder pain• Prevents recurrent dislocation• Maintains proper joint alignment• Promotes safe tissue healing These benefits are most effective when the shoulder immobilizer is worn consistently as prescribed. When Doctors Recommend a Shoulder Immobilizer Doctors commonly recommend a shoulder immobilizer as part of conservative or post-operative treatment for joint injuries and instability. Medical situations where doctors may recommend it: • After shoulder dislocation• Following rotator cuff repair• During severe shoulder instability• Post-fracture stabilization• Acute left shoulder pain causes A shoulder immobilizer is usually advised before gradually transitioning into shoulder stretching exercises and later a full shoulder workout. Non-Surgical TreatmentTransition to Shoulder Stretching Exercises Once the initial healing phase is complete and pain is under control, gradual movement becomes essential to prevent joint stiffness and muscle tightness. Controlled motion helps restore flexibility and prepares the shoulder for strengthening. Shoulder stretching exercises may include: • Pendulum arm movements• Assisted with wall climbing• Gentle external rotations• Passive range-of-motion drills These controlled shoulder stretching exercises gradually restore flexibility, improve range of motion, reduce stiffness, and safely rebuild mobility after shoulder immobilizer use under proper medical supervision. Full Shoulder Workout After Recovery After the healing phase is complete and pain is well controlled, gradual strengthening exercises are essential to restore shoulder stability, improve muscle balance, and prevent recurrent shoulder instability. A full shoulder workout may include: • Rotator cuff strengthening• Resistance band exercises• Scapular stabilization drills• Light dumbbell movements A structured full shoulder workout rebuilds strength, improves stability, restores movement control, and reduces future shoulder instability after prolonged immobilization. How to Choose the Right Shoulder Immobilizer Choosing the right shoulder immobilizer depends on the type of injury, stability requirement, recovery stage, and comfort needs. Proper selection ensures effective joint support and prevents complications during healing. Key factors to consider: • Severity of injury and instability level• Requirement of additional torso strap support• Comfort, fit, and adjustability features• Breathable and skin-friendly material design• Doctor’s recommendation and medical guidance Injury severity, proper fit, breathable material, and medical advice are essential when selecting a shoulder immobilizer to ensure correct alignment, stability, comfort, and safe recovery. How to Use a Shoulder Immobilizer Correctly Correct usage of a shoulder immobilizer is essential to ensure proper joint stabilization, prevent complications, and support safe tissue healing during the recovery period Best practices include: • Wear it exactly as prescribed by your doctor• Do not remove without medical advice• Keep elbow positioned at 90 degrees• Ensure shoulder remains close to body• Keep straps secure but not overly tight• Remove only during approved exercises• Maintain proper hygiene under brace• Attend scheduled follow-up visits A shoulder immobilizer should be worn continuously during the initial healing phase unless your doctor advises otherwise. Removing it too early may increase the risk of shoulder instability or delayed recovery. FAQs – Shoulder Immobilizer What is the difference between a sling and a shoulder immobilizer? A sling supports the forearm, while
Locking and Unlocking of Knee Joint: Causes, Symptoms & Treatment
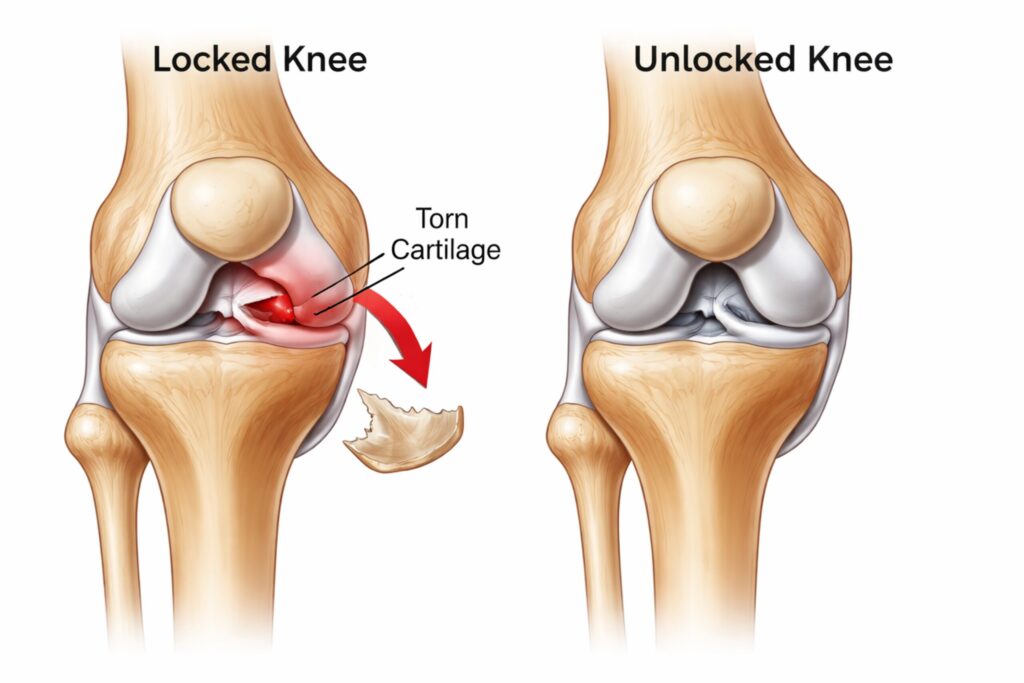
Locking and Unlocking of Knee Joint: Causes, Symptoms & Treatment The locking and unlocking of the knee joint is a condition that can significantly interfere with daily activities such as walking, climbing stairs, squatting, or even standing for long periods. Many patients describe it as a sudden “stuck” feeling in the knee joint, where the knee refuses to bend or straighten completely. Sometimes it unlocks suddenly with a click or pop, often accompanied by discomfort or instability. Understanding the locking and unlocking of the knee joint requires knowledge of knee structure, biomechanics, injury patterns, and available treatment options. In this comprehensive and user-friendly guide, we will discuss the anatomy, causes, symptoms, diagnosis, and management of this condition in detail. What Is Locking and Unlocking of Knee Joint? The locking and unlocking of knee joint refers to a mechanical or functional disturbance in which the knee becomes temporarily fixed in one position. It may remain bent (flexed) or straight (extended) and require effort, manipulation, or movement to return to normal motion. There are two main types: 1. True Locking True locking occurs when something physically blocks normal knee joint movement, such as a torn cartilage fragment. 2. Pseudo Locking Pseudo locking occurs due to severe knee joint pain, swelling, or muscle spasm without a structural blockage. To understand this better, it is important to answer the question: What type of joint is the knee? The knee is a modified hinge joint. While it primarily allows bending and straightening, it also permits slight rotation. This rotational movement is essential for the natural locking and unlocking of knee joint mechanism. Knee Joint Anatomy: Understanding the Structure A clear understanding of knee joint anatomy helps explain why the locking and unlocking of knee joint occurs. The knee joint consists of three major bones: Femur (thigh bone) Tibia (shin bone) Patella (kneecap) These bones are supported by strong knee joint ligaments, including: Anterior Cruciate Ligament (ACL) Posterior Cruciate Ligament (PCL) Medial Collateral Ligament (MCL) Lateral Collateral Ligament (LCL) These ligaments maintain stability and guide proper knee joint movement. Additionally, the menisci (medial and lateral) act as shock absorbers between the femur and tibia. Smooth cartilage covers bone surfaces to reduce friction. If any part of this complex knee joint anatomy is injured, the natural locking and unlocking of knee joint process can be disrupted. How the Locking and Unlocking of Knee Joint Works The normal locking and unlocking of knee joint occur during full extension and flexion. This is known as the “screw-home mechanism. Locking Phase As the knee straightens fully, the tibia rotates slightly outward. The knee joint ligaments tighten. The joint becomes stable for standing. Unlocking Phase The popliteus muscle rotates the tibia inward. The ligaments relax slightly. The knee bends smoothly. When this mechanism is impaired due to injury or degeneration, abnormal locking and unlocking of knee joint episodes may occur. Common Causes of Locking and Unlocking of Knee Joint Several orthopedic conditions can cause abnormal locking and unlocking of knee joint: 1. Meniscus Tear A torn meniscus is one of the most common causes. A displaced cartilage fragment may block normal knee joint movement, leading to sudden locking. Symptoms include: Sharp knee joint pain Swelling Clicking sensation Inability to fully extend the knee 2. Ligament Injuries Damage to knee joint ligaments, especially ACL injuries, can cause instability. This instability may alter the normal locking and unlocking of the knee joint. 3. Loose Bodies Small fragments of bone or cartilage floating inside the knee joint can interfere with movement, causing unpredictable locking episodes. 4. Osteoarthritis Degeneration of cartilage affects knee joint anatomy, leading to rough surfaces and mechanical catching. This may disturb the locking and unlocking of knee joint. 5. Patellar Maltracking Improper alignment of the kneecap may cause abnormal pressure distribution, contributing to knee joint pain and disturbed movement patterns. Symptoms of Locking and Unlocking of Knee Joint Patients experiencing locking and unlocking of knee joint commonly report: Sudden inability to bend or straighten the knee A popping or clicking sound Swelling in the knee joint Recurrent knee joint pain Feeling of instability Sensation of something stuck inside If symptoms are frequent or worsening, professional evaluation is essential. Diagnosis of Locking and Unlocking of Knee Joint Accurate diagnosis is important for proper treatment. Clinical Examination The doctor evaluates: Range of motion Stability of knee joint ligaments Tenderness and swelling Pain during knee joint movement Imaging Tests X-Ray Checks bone alignment and arthritis changes. MRI Provides detailed information about: Meniscus tears Ligament injuries Cartilage damage Structural abnormalities affecting locking and unlocking of knee joint MRI is especially helpful in evaluating soft tissue structures within the knee joint anatomy. Non-Surgical Treatment Mild or early cases of locking and unlocking of knee joint can often be treated conservatively. 1. Rest and Activity Modification Avoid activities that worsen symptoms. 2. Ice Therapy Reduces swelling and inflammation. 3. Medications Anti-inflammatory drugs help relieve knee joint pain. 4. Physiotherapy A structured rehabilitation program improves: Muscle strength Stability of knee joint ligaments Range of knee joint movement Strengthening quadriceps and hamstrings supports proper locking and unlocking of knee joint function. Surgical Treatment If mechanical blockage persists, surgery may be required. Arthroscopic Surgery A minimally invasive procedure used to: Repair torn meniscus Remove loose bodies Reconstruct damaged knee joint ligaments Smooth cartilage surfaces Arthroscopy effectively restores normal locking and unlocking of the knee joint mechanics in many patients. Recovery time varies depending on the procedure but generally ranges from a few weeks to several months. Rehabilitation and Recovery Proper rehabilitation is essential after treatment for the locking and unlocking of the knee joint. Rehabilitation focuses on: Gradual restoration of knee joint movement Strengthening surrounding muscles Improving balance and coordination Reducing the recurrence of knee joint pain Adherence to physiotherapy significantly improves outcomes. Prevention of Locking and Unlocking of Knee Joint Preventive strategies include: Maintaining a healthy body weight Strength training for lower limb muscles Warm-up before sports Avoiding sudden twisting movements Early treatment of ligament injuries Healthy knee
How to Speed Up Muscle Strain Recovery in Athletes

How to Speed Up Muscle Strain Recovery in Athletes Muscle injuries are one of the most common problems athletes face. Whether you are a professional player or a fitness enthusiast, a muscle strain can interrupt training, reduce performance, and delay competition plans. Many athletes search for how to speed up muscle strain recovery because they want to return to sports safely and quickly. The truth is, recovery cannot be rushed artificially, but it can be optimized with the right approach. This guide explains the healing process, recovery stages, rehabilitation principles, and safe return-to-play strategies in a structured and easy-to-understand format. Understanding Muscle Strain in Athletes A muscle strain occurs when muscle fibers are overstretched or torn due to sudden force or excessive load. This commonly happens during sprinting, jumping, rapid direction changes, or heavy lifting. Muscle strains are classified into three grades. Mild strains involve microscopic damage and cause slight discomfort. Moderate strains include partial tears and noticeable weakness. Severe strains involve complete tears and significant loss of muscle function. Athletes frequently experience strains in the hamstrings, quadriceps, calves, and lower back. A muscle strain in back often develops due to improper lifting mechanics or weak core stability. Similarly, an abdominal muscle strain is common in sports that involve twisting movements, such as cricket, tennis, and throwing events. Understanding the severity of injury is the first step toward knowing how to heal muscle strain effectively. The Healing Process: What Happens Inside the Muscle To understand how to speed up muscle strain recovery, it is important to know how muscles heal. Muscle healing occurs in three main phases: 1. Inflammatory Phase (First 72 Hours) The body sends blood and immune cells to the injured area. Swelling and pain are common during this stage. This is a protective response. 2. Repair Phase (3 Days to 3 Weeks) New muscle fibers begin forming. Collagen develops to rebuild damaged tissue. 3. Remodeling Phase (3 Weeks and Beyond) The new tissue becomes stronger and more organized. Gradual strengthening is essential during this phase. If rehabilitation is not structured properly, scar tissue may form incorrectly, increasing the risk of re-injury. Early Management: The First 72 Hours Matter The initial phase determines how quickly and safely recovery progresses. During the first 48–72 hours, the goal is to control inflammation. Rest is important, but complete immobility should be avoided unless the injury is severe. Ice application for short intervals helps reduce swelling and pain. Compression and elevation may further assist in controlling inflammation. This early care forms the foundation of how to treat muscle strain safely and effectively. When and How to Start Movement Many athletes make the mistake of either returning too early or resting for too long. Both can delay healing. After the initial inflammatory phase, gentle, pain-free movement should begin. Controlled activation improves blood circulation and supports proper alignment of healing fibers. Light stretching without pain, simple mobility exercises, and isometric contractions can help restore muscle function. For example, in a muscle strain in back, controlled core activation and posture correction exercises support recovery. In an abdominal muscle strain, breathing exercises and gentle trunk stabilization are helpful during early stages. This balanced approach is essential for those wondering how to cure muscle strain efficiently. Strengthening Phase: Building Back Muscle Capacity Once pain reduces and movement improves, strengthening becomes critical. Muscles heal stronger when gradually exposed to controlled resistance. At this stage, light resistance exercises, band training, and progressive loading are introduced. Eccentric strengthening is particularly beneficial because it improves muscle control and resilience. Athletes must avoid aggressive stretching or heavy loading too soon. Progressive strengthening ensures safe tissue remodeling and reduces recurrence risk. If someone asks how to heal muscle strain completely, the answer always includes structured strengthening, not just rest. The Role of Nutrition in Faster Recovery Nutrition plays a significant role in muscle repair. Protein supports muscle fiber regeneration. Athletes recovering from a muscle strain should ensure adequate daily protein intake from balanced sources. Hydration is equally important because fluid balance supports circulation and cellular repair. Anti-inflammatory nutrients such as omega-3 fatty acids, leafy vegetables, and antioxidant-rich foods can support the healing process. However, nutrition works best when combined with proper rehabilitation. Sleep and Hormonal Recovery Sleep is often underestimated in injury recovery. During deep sleep, growth hormone secretion increases, accelerating tissue repair. Athletes should prioritize 7–9 hours of quality sleep during the healing period. Without proper rest, even the best rehabilitation program may not deliver optimal results. Special Considerations for Back and Abdominal Strains A muscle strain in back requires attention to posture, hip mobility, and core strength. Weak supporting muscles can overload the lower back, delaying recovery. An abdominal muscle strain requires gradual progression in rotational movements. Sudden twisting or aggressive core workouts too early can worsen the injury. These specific adjustments are essential when considering how to speed up muscle strain recovery in athletes participating in rotational or lifting sports. Safe Return to Sports Returning too early is one of the most common reasons for re-injury. Before returning to full training, the athlete should have: Full pain-free range of motion Nearly equal strength compared to the uninjured side Ability to perform sport-specific drills without discomfort No swelling after practice sessions Gradual return-to-play progression ensures long-term success. Common Mistakes That Delay Recovery Many athletes unknowingly slow down recovery by: Ignoring mild pain Skipping rehabilitation exercises Returning to competition too soon Not correcting training errors Overstretching in the early stages Understanding these mistakes is part of knowing how to treat muscle strain correctly. Realistic Recovery Timeline Recovery depends on severity. Mild strains may heal within one to two weeks. Moderate injuries typically require three to six weeks. Severe tears may take several months and sometimes need medical supervision. Patience combined with structured rehabilitation is the safest path forward. FAQs How long does a muscle strain usually take to heal? Mild strains heal within 1–2 weeks, moderate injuries may take 3–6 weeks, and severe tears can require several months. What
Shoulder Bone Fracture Treatment: Symptoms and Care
Shoulder Bone Fracture Treatment: Symptoms and Care A shoulder injury can be painful and frightening, especially when it involves a broken bone. Understanding shoulder bone fracture treatment is important so that patients receive timely care, avoid complications, and return to normal activities safely. The shoulder is a complex joint made up of bones, ligaments, tendons, and muscles. When any part of this structure is damaged, movement and daily function can be affected. In this detailed guide, you will learn about symptoms, causes, diagnosis, treatment options, recovery process, and related conditions such as shoulder ligament injuries and frozen shoulder. The goal is to provide clear, easy-to-understand, and medically accurate information. What Is a Shoulder Bone Fracture? A shoulder bone fracture occurs when one of the bones in the shoulder region breaks due to trauma or excessive force. The shoulder consists of three main bones: Clavicle (collarbone) Scapula (shoulder blade) Proximal humerus (upper arm bone) A fracture can occur in any of these bones, but clavicle and proximal humerus fractures are most common. Immediate shoulder bone fracture treatment is necessary to reduce pain, ensure proper bone alignment, and prevent long-term stiffness or deformity. Common Causes of Shoulder Bone Fracture Understanding the cause helps doctors decide the right shoulder fracture treatment plan. 1. Road Traffic Accidents High-impact injuries from bike or car accidents are a major cause. 2. Sports Injuries Falls during cricket, football, kabaddi, or gym workouts may lead to fractures. 3. Fall on an Outstretched Arm This is common in elderly patients. 4. Osteoporosis Weak bones increase fracture risk, especially in older adults. Early diagnosis ensures proper shoulder bone fracture treatment and faster healing. Symptoms of Shoulder Bone Fracture Recognizing symptoms quickly helps prevent complications. Severe Shoulder Pain Intense shoulder pain immediately after injury. Swelling and Bruising Visible swelling around the shoulder joint. Limited Movement Difficulty lifting the arm. Deformity In some cases, the shoulder may look uneven or displaced. If you experience these symptoms, seek immediate medical care. Diagnosis of Shoulder Bone Fracture Doctors use the following methods: Physical Examination Checking swelling, tenderness, and movement restriction. X-Ray Confirms the location and severity of the fracture. CT Scan Used in complex fractures for surgical planning. Proper diagnosis guides the correct shoulder bone fracture treatment strategy. Types of Shoulder Bone Fractures Treatment depends on fracture type. Non-Displaced Fracture Bone remains aligned. Usually shown to be stable on X-ray. Displaced Fracture Bone fragments are separated. Comminuted Fracture The bone breaks into multiple pieces. Each type requires a different shoulder fracture treatment approach. Shoulder Bone Fracture Treatment Options The method of shoulder bone fracture treatment depends on severity, patient age, and activity level. Non-Surgical Shoulder Bone Fracture Treatment Many shoulder fractures heal without surgery. Sling Immobilization Arm is supported in a sling for 3–6 weeks. Pain Management Medications to control shoulder pain. Physiotherapy Gentle exercises after initial healing to prevent stiffness. Non-surgical treatment is common in minor fractures and elderly patients. Surgical Shoulder Bone Fracture Treatment Surgery may be required when: Bones are severely displaced Fracture involves joint surface Multiple bone fragments exist Surgical Methods Plate and screw fixation Rod fixation Shoulder replacement (in severe cases) Surgery ensures stable bone healing and better long-term function. Recovery Timeline After Shoulder Bone Fracture Healing usually takes 6 to 12 weeks, depending on severity. First 2 Weeks Pain and swelling control. 3–6 Weeks Gradual arm movement exercises. 6–12 Weeks Strength training and physiotherapy. Following the correct shoulder bone fracture treatment plan improves outcomes. Shoulder Fracture Treatment vs Shoulder Ligament Tear Treatment Sometimes a fracture is accompanied by soft tissue damage. Shoulder Fracture Treatment Bone break due to fall or trauma Managed with sling, medicines, or surgery Focus on proper bone healing Shoulder Ligament Tear Treatment Ligament injury affects joint stability Treated with rest and physiotherapy Severe cases may need arthroscopic repair Both conditions require accurate diagnosis for complete shoulder recovery. Frozen Shoulder After Fracture Some patients develop stiffness after injury or surgery. What Is Frozen Shoulder? Frozen shoulder causes pain and restricted movement. Frozen Shoulder Treatment Options Physiotherapy Anti-inflammatory medications Joint injections In rare cases, arthroscopic release Early rehabilitation reduces the risk of needing best treatment for frozen shoulder later. Managing Shoulder Pain During Recovery Persistent shoulder pain can delay healing. Tips: Follow doctor’s instructions Avoid heavy lifting Attend regular physiotherapy Use ice packs as advised Pain gradually decreases as healing progresses. Complications If Not Treated Properly Ignoring or delaying shoulder bone fracture treatment may lead to: Permanent stiffness Malunion (improper bone healing) Chronic shoulder pain Joint arthritis Muscle weakness Timely care prevents these issues. Prevention Tips for Shoulder Injuries Wear protective sports gear Maintain bone strength with calcium Improve balance to prevent falls Strengthen shoulder muscles Prevention is always better than long-term treatment. When to See an Orthopedic Specialist Consult a specialist if: Pain is severe Movement is limited Swelling increases Deformity is visible Early orthopedic evaluation ensures correct shoulder fracture treatment and better recovery. FAQs How long does shoulder bone fracture treatment take? Healing usually takes 6–12 weeks, but full recovery may take 3–4 months with physiotherapy. Can shoulder fractures heal without surgery? Yes, many fractures heal with sling support and physiotherapy. What is the best treatment for frozen shoulder after fracture? The best treatment for frozen shoulder includes physiotherapy, medication, and sometimes joint injections. Is shoulder pain normal after fracture healing? Mild discomfort is normal during recovery, but severe or persistent pain should be evaluated. What is the difference between shoulder ligament tear treatment and fracture treatment? Fracture treatment focuses on bone healing, while shoulder ligament tear treatment repairs soft tissue structures. Conclusion A shoulder injury should never be ignored. Proper shoulder bone fracture treatment ensures correct healing, reduces pain, and restores full movement. Early diagnosis, structured rehabilitation, and expert orthopedic care are key to successful recovery. Understanding symptoms, following medical advice, and completing physiotherapy are essential steps toward regaining shoulder strength and function. If you experience persistent shoulder pain or limited movement after injury, seek medical evaluation immediately.
ACL Surgery Cost in India for Sports Injury Treatment
ACL Surgery Cost in India for Sports Injury Treatment Sports injuries are increasingly common among professional athletes, fitness enthusiasts, and even recreational players. One of the most serious knee injuries is an ACL tear. If you or someone in your family has been advised surgery, the first question that usually comes to mind is about ACL surgery cost. This detailed guide explains ACL surgery pricing in India, treatment options, recovery expectations, and important medical considerations. The objective is to provide clarity so patients can make informed healthcare decisions. Understanding ACL Injury and Why Surgery Is Needed The Anterior Cruciate Ligament (ACL) is one of the key stabilizing ligaments in the knee joint. It connects the femur (thigh bone) to the tibia (shin bone) and prevents excessive forward movement and rotation. An ACL tear commonly occurs during: Football Cricket Basketball Kabaddi Sudden twisting injuries Road accidents A complete ACL tear often requires ACL surgery because the ligament does not heal naturally. Without surgical reconstruction, patients may experience instability, repeated knee giving-way episodes, and long-term cartilage damage. ACL Surgery Cost in India – Complete Breakdown When discussing ACL surgery cost, it is important to understand that pricing varies based on hospital type, city, surgeon expertise, implant quality, and rehabilitation services. Average ACL Surgery Cost in India In India, the ACL surgery cost typically ranges between: ₹1,20,000 to ₹3,50,000 in private hospitals ₹60,000 to ₹1,20,000 in government hospitals Metro cities like Delhi NCR, Mumbai, and Bangalore generally have slightly higher costs due to infrastructure and specialist availability. Factors That Affect ACL Surgery Cost Several medical and non-medical factors influence ACL surgery cost: Hospital Category – NABH-accredited hospitals may charge more. Surgeon’s Expertise – Experienced arthroscopic surgeons may have higher fees. Implant Type – Bio-absorbable screws, titanium implants, or imported graft fixation systems can increase cost. Room Category – General ward vs private or deluxe rooms. Additional Injuries – Meniscus repair or cartilage procedures increase expense. Rehabilitation Cost – Physiotherapy sessions after surgery. Understanding these components helps patients estimate the total financial commitment. Types of ACL Surgery and Their Cost Impact The types of ACL surgery also influence pricing and recovery. Arthroscopic ACL Reconstruction This is the most common method. It is minimally invasive and performed using a camera (arthroscope). Faster recovery Smaller incisions Reduced hospital stay Most modern ACL surgery cost calculations are based on arthroscopic techniques. Autograft vs Allograft Surgery Autograft Surgery – Uses the patient’s own tendon (hamstring or patellar tendon). Allograft Surgery – Uses donor tissue. Autografts are more common in India and relatively cost-effective. Allografts may increase ACL surgery cost due to graft procurement charges. Detailed Expense Structure of ACL Surgery To understand ACL surgery cost clearly, here is a breakdown: 1. Pre-Surgery Expenses MRI scan Blood tests Orthopedic consultation 2. Surgical Charges Operation theatre charges Surgeon fees Anesthesia charges 3. Implant & Graft Cost This is one of the biggest components affecting ACL surgery cost. 4. Hospital Stay Usually 1–3 days. 5. Post-Surgery Physiotherapy Rehabilitation is crucial for full knee recovery. ACL Surgery Recovery Time – What to Expect A common concern apart from ACL surgery cost is ACL surgery recovery time. Recovery typically progresses in stages: First 2 Weeks Swelling reduction Pain management Gentle range-of-motion exercises 1 to 3 Months Strength-building exercises Partial return to normal walking 4 to 6 Months Light jogging Agility training 6 to 9 Months Return to sports (depending on rehabilitation progress) Athletes may require structured physiotherapy programs to ensure safe return to play. ACL Tear Surgery Procedure Explained During ACL tear surgery, the torn ligament is removed and replaced with a graft. The surgeon drills small tunnels in the tibia and femur to fix the new ligament securely. The surgery usually takes 60–90 minutes and is done under spinal or general anesthesia. Most patients are discharged within 24–48 hours. Bad Signs After ACL Surgery – When to Consult a Doctor While ACL surgery is generally safe, patients should be aware of potential complications. Warning Signs Include: Persistent high fever Excessive swelling Redness or discharge from incision Severe calf pain Limited knee movement beyond expected levels Recognizing these bad signs after ACL surgery early can prevent serious complications. Is ACL Surgery Covered by Insurance? Many health insurance policies in India cover ACL surgery cost under hospitalization benefits. However: Waiting period may apply Pre-existing injury clauses may affect coverage Sub-limits on implants may exist Patients should check policy terms before admission. Why Timely ACL Surgery Is Important for Athletes Ignoring ACL injury can lead to: Repeated knee instability Meniscus damage Early osteoarthritis Reduced sports performance For athletes and active individuals, early intervention reduces long-term damage and improves functional outcomes. How to Reduce ACL Surgery Cost Patients can manage ACL surgery cost by: Comparing hospital packages Choosing in-network insurance hospitals Opting for standard room categories Confirming implant pricing in advance Checking cashless insurance options Transparent financial planning prevents unexpected expenses. Long-Term Outcome After ACL Surgery Most patients regain normal knee function with proper rehabilitation. Success rates are high when surgery is performed by experienced orthopedic surgeons. Key to success: Structured physiotherapy Muscle strengthening Avoiding premature sports return Regular follow-ups FAQs What is the average ACL surgery cost in India? The ACL surgery cost in India ranges between ₹1,20,000 and ₹3,50,000 in private hospitals depending on surgeon, hospital, and implant type. What is ACL surgery recovery time? ACL surgery recovery time typically ranges from 6 to 9 months for full return to sports activities. What are the types of ACL surgery? The main types of ACL surgery include arthroscopic ACL reconstruction, autograft reconstruction, and allograft reconstruction. How long does ACL tear surgery take? ACL tear surgery generally takes 60 to 90 minutes, and patients are discharged within 1–2 days. What are bad signs after ACL surgery? Bad signs after ACL surgery include fever, excessive swelling, redness, wound discharge, severe pain, and restricted knee movement. Conclusion Understanding ACL surgery cost in India for sports injury treatment is essential for financial
ACL Reconstruction सर्जरी के बाद कितने समय में सामान्य चलना और खेलना संभव है?
ACL Reconstruction सर्जरी के बाद कितने समय में सामान्य चलना और खेलना संभव है? ACL Reconstruction Surgery घुटने की एक महत्वपूर्ण शल्य प्रक्रिया है, जो तब की जाती है जब ACL लिगामेंट पूरी तरह या गंभीर रूप से फट जाता है। ACL घुटने के चार प्रमुख लिगामेंट्स में से एक है, जो घुटने को स्थिरता प्रदान करता है और आगे-पीछे तथा घुमावदार गति को नियंत्रित करता है। खेल के दौरान अचानक मुड़ना, गलत तरीके से उतरना, सड़क दुर्घटना या तेज झटका लगने से ACL चोट हो सकती है। ऐसे में अक्सर मरीज का सबसे बड़ा प्रश्न होता है — ACL Reconstruction सर्जरी के बाद सामान्य चलना और खेलना कब संभव होगा? इस लेख में हम ACL सर्जरी रिकवरी समय, ACL टियर सर्जरी, ACL सर्जरी के प्रकार, ACL सर्जरी के बाद खराब संकेत और संपूर्ण पुनर्वास प्रक्रिया को विस्तार से समझेंगे। ACL लिगामेंट क्या है और इसकी भूमिका क्यों महत्वपूर्ण है? ACL (Anterior Cruciate Ligament) जांघ की हड्डी और पिंडली की हड्डी को जोड़ने वाला प्रमुख लिगामेंट है। यह घुटने को स्थिरता देता है, आगे खिसकने से रोकता है और अचानक मुड़ने या दिशा बदलने के दौरान संतुलन बनाए रखता है, जिससे चलना, दौड़ना और कूदना सुरक्षित रहता है। घुटने को आगे की ओर खिसकने से रोकना घुटने की घुमावदार स्थिरता बनाए रखना अचानक दिशा बदलते समय संतुलन देना यदि यह लिगामेंट फट जाए, तो घुटना अस्थिर महसूस होता है, बार-बार मुड़ सकता है और सामान्य चलना भी कठिन हो जाता है। ACL टियर सर्जरी कब आवश्यक होती है? जब ACL पूरी तरह फट जाता है, तो घुटने में अस्थिरता, अचानक मुड़ जाना, सूजन, दर्द और चलने-दौड़ने में कठिनाई जैसी समस्याएँ दिखाई देती हैं। ऐसे मामलों में घुटना सामान्य गतिविधियों के दौरान भी साथ नहीं देता और बार-बार लड़खड़ाने का अनुभव होता है, तब शल्य उपचार की आवश्यकता पड़ सकती है। चलते समय घुटना मुड़ जाना बार-बार सूजन आना खेल या दौड़ने में असमर्थता एमआरआई में पूर्ण टियर दिखाई देना तब डॉक्टर ACL टियर सर्जरी की सलाह देते हैं। यह सर्जरी घुटने की स्थिरता बहाल करने के लिए की जाती है। ACL सर्जरी के प्रकार ACL सर्जरी के प्रकार मुख्यतः उपयोग किए गए ग्राफ्ट पर आधारित होते हैं। 1. स्वयं के शरीर से ग्राफ्ट (ऑटोग्राफ्ट तकनीक) इसमें मरीज के हैमस्ट्रिंग या पाटेला टेंडन का उपयोग किया जाता है। यह सबसे अधिक प्रचलित और सुरक्षित तरीका माना जाता है। 2. डोनर ग्राफ्ट (एलोग्राफ्ट तकनीक) इसमें किसी डोनर से प्राप्त टेंडन का उपयोग किया जाता है। यह उन मरीजों के लिए उपयुक्त है जिन्हें कम आक्रामक प्रक्रिया चाहिए। 3. आधुनिक आर्थ्रोस्कोपिक तकनीक आज अधिकांश ACL Reconstruction Surgery आर्थ्रोस्कोपी द्वारा की जाती है, जिसमें छोटे चीरे लगाए जाते हैं और रिकवरी तेज होती है। ACL सर्जरी रिकवरी समय ACL सर्जरी के बाद ठीक होने का समय मरीज की उम्र, शारीरिक स्थिति, अपनाई गई शल्य तकनीक और पुनर्वास कार्यक्रम पर निर्भर करता है। सामान्यतः रिकवरी को अलग-अलग चरणों में बाँटा जाता है। पहला चरण (0–2 सप्ताह) सूजन और दर्द नियंत्रण घुटने को सीधा रखने के व्यायाम बैसाखी की सहायता से चलना हल्की फिजियोथेरेपी शुरू दूसरा चरण (3–6 सप्ताह) बिना सहारे धीरे-धीरे चलना मांसपेशियों को मजबूत बनाना घुटने को 120 डिग्री तक मोड़ना तीसरा चरण (2–4 महीने) संतुलन और स्थिरता व्यायाम हल्की जॉगिंग सीढ़ियाँ सामान्य रूप से चढ़ना चौथा चरण (5–9 महीने) खेल संबंधित अभ्यास दिशा बदलने वाले व्यायाम पूर्ण खेल गतिविधि की तैयारी अधिकांश मरीजों में 6 से 9 महीने में खेल में वापसी संभव होती है। ACL सर्जरी के बाद सामान्य चलना कब संभव है? 1–2 सप्ताह में सहारे से चलना 4–6 सप्ताह में सामान्य चलना 3 महीने में बिना दर्द और आत्मविश्वास के साथ चलना ACL सर्जरी के बाद खेल कब शुरू करें? घुटने में सूजन न हो मांसपेशियों की ताकत 90% तक वापस आ जाए संतुलन परीक्षण पास हो डॉक्टर और फिजियोथेरेपिस्ट की अनुमति आमतौर पर 6–9 महीने बाद प्रतिस्पर्धात्मक खेल संभव होता है, लेकिन यह पूरी तरह मरीज की रिकवरी, मांसपेशियों की ताकत, संतुलन और डॉक्टर की अनुमति पर निर्भर करता है। यदि फिजियोथेरेपी सही तरीके से पूरी की गई हो और घुटने में कोई सूजन या दर्द न हो, तभी सुरक्षित रूप से खेल में वापसी करनी चाहिए, ताकि दोबारा चोट लगने का खतरा कम हो सके। ACL सर्जरी के बाद खराब संकेत लगातार बढ़ती सूजन तेज दर्द जो कम न हो घाव से पस निकलना बुखार घुटने में असामान्य ढीलापन ये ACL सर्जरी के बाद दिखाई देने वाले गंभीर और चिंताजनक संकेत हो सकते हैं, इसलिए ऐसी स्थिति में तुरंत किसी विशेषज्ञ डॉक्टर से चिकित्सकीय सलाह लेना बेहद आवश्यक होता है। क्या बिना सर्जरी ACL ठीक हो सकता है? आंशिक टियर में कुछ मामलों में बिना सर्जरी उपचार संभव है, लेकिन पूर्ण टियर में ACL Reconstruction Surgery ही स्थायी समाधान मानी जाती है। FAQ (अक्सर पूछे जाने वाले प्रश्न) एसीएल सर्जरी के बाद पूरी तरह ठीक होने में कितना समय लगता है? सामान्यतः 6–9 महीने, लेकिन यह व्यक्ति की शारीरिक स्थिति और व्यायाम अनुशासन पर निर्भर करता है। क्या एसीएल सर्जरी के बाद दोबारा चोट लग सकती है? हाँ, यदि पुनर्वास अधूरा हो या जल्दबाजी में खेल शुरू किया जाए। क्या एसीएल सर्जरी के बाद दौड़ना सुरक्षित है? डॉक्टर की अनुमति के बाद 3–4 महीने में हल्की दौड़ शुरू की जा सकती है। एसीएल सर्जरी के बाद खराब संकेत कौन से हैं? लगातार सूजन, तेज दर्द, संक्रमण और घुटने की अस्थिरता। क्या सभी एसीएल टियर में सर्जरी जरूरी होती है? नहीं, आंशिक टियर में कुछ मामलों में बिना सर्जरी उपचार संभव है। निष्कर्ष ACL Reconstruction Surgery के बाद सामान्य चलना लगभग 4–6 सप्ताह में संभव हो सकता है, जबकि खेल गतिविधियों में पूरी तरह वापसी के लिए 6–9 महीने का समय लग सकता है। सही समय पर ACL टियर सर्जरी, उचित ACL सर्जरी तकनीक का चयन, और अनुशासित पुनर्वास कार्यक्रम ही सफल परिणाम की कुंजी हैं। यदि आप सुरक्षित और सफल ACL सर्जरी करवाना चाहते हैं, तो Dr. Himanshu Gupta एक अनुभवी और कुशल ऑर्थोपेडिक सर्जन हैं, जिन्हें ACL Reconstruction Surgery और स्पोर्ट्स इंजरी उपचार में विशेष विशेषज्ञता प्राप्त है। उनकी उन्नत आर्थ्रोस्कोपिक तकनीक और संरचित पुनर्वास मार्गदर्शन मरीजों को तेज, सुरक्षित और स्थायी रिकवरी में मदद करता
Partial ACL Tear: Symptoms, Causes, Treatment & Recovery Guide

Partial ACL Tear: Symptoms, Causes, Treatment & Recovery Guide A partial ACL tear is a common knee ligament injury in which the anterior cruciate ligament is damaged but not completely ruptured. The ACL plays an essential role in stabilizing the knee joint, supporting movement, and preventing excessive forward motion of the shin bone. When some fibers of the ligament are injured, patients may still be able to walk but often experience pain, instability, and reduced performance during physical activity. People searching for information about partial ACL tear symptoms, treatment, MRI diagnosis, and partial ACL tear recovery time without surgery usually want clear guidance on healing options and long-term outcomes. Understanding whether do partial ACL tears heal, how rehabilitation works, and when to use a knee brace for ACL tear helps patients make informed treatment decisions. This comprehensive guide explains what a partial ACL tear is, its symptoms, MRI diagnosis, treatment options, recovery process, long-term effects without surgery, and answers common patient questions in a simple and human-friendly way. What Is a Partial ACL Tear? A partial ACL tear is a condition in which the anterior cruciate ligament is only partially torn, allowing the knee to retain some stability. Despite limited fiber damage, patients may experience pain, swelling, and functional difficulty, especially during twisting movements or sports. Key Features of Partial ACL Tear Partial loss of knee stability: The knee may feel weak, especially during sudden pivoting or turning motions. Swelling and tenderness: Inflammation develops around the joint, causing discomfort and limited movement. Pain during activity: Walking, running, or climbing stairs may trigger moderate knee pain. Reduced range of motion: Bending and straightening the knee can be stiff and limited. Partial ACL tears require proper assessment to restore knee function and prevent long-term instability or secondary injuries. Symptoms of Partial ACL Tear Symptoms of a partial ACL tear may be subtle initially but tend to worsen with physical activity. Early identification of signs can improve recovery outcomes and prevent further knee damage. Common Symptoms Include Knee pain during activity: Moderate discomfort often increases when twisting or landing from jumps. Swelling within 24 hours: The knee may swell due to internal bleeding or fluid accumulation. Feeling of instability: The joint may “give way” unexpectedly during walking or running. Difficulty performing movements: Daily activities like climbing stairs or squatting can be challenging. Recognizing these symptoms early supports effective rehabilitation and minimizes long-term knee complications. Causes of Partial ACL Tear A partial ACL tear can result from various injuries or movements that strain the ligament fibers, particularly in sports or high-impact activities. Understanding causes helps in prevention and treatment. Common Causes Include Sudden directional changes: Quick pivoting during sports can overstretch the ACL fibers. Direct impact on the knee: Collisions or falls may partially tear the ligament. Landing awkwardly from jumps: Poor landing technique increases ligament stress and risk of tearing. Overstretching the knee: Excessive bending or twisting beyond normal limits can cause fiber damage. Preventing high-risk movements and strengthening surrounding muscles reduces the likelihood of partial ACL tears. How Partial ACL Tear Diagnosed Diagnosis of a partial ACL tear is essential to distinguish it from a complete rupture and to determine the best treatment approach for optimal recovery. Diagnostic Methods Physical examination tests: Lachman and pivot-shift tests assess ligament stability and knee function. Partial ACL tear MRI: Provides detailed images of ligament fibers to confirm the extent of the tear. X-rays: Help rule out fractures or associated bone injuries. Early and accurate diagnosis ensures proper treatment and reduces the risk of chronic knee instability. Treatment Options for Partial ACL Tear Treatment for a partial ACL tear depends on severity, activity level, and knee stability, with many cases responding well to non-surgical care. Non-Surgical Treatment Rest and activity modification: Limiting strenuous movements helps damaged fibers heal properly. Ice therapy: Reduces swelling and alleviates discomfort in the injured knee. Pain medications: Over-the-counter drugs may help manage moderate knee pain effectively. Knee brace for ACL tear: Stabilizes the knee and prevents additional ligament strain. Physical therapy exercises: Strengthens muscles and improves overall knee function safely. Most partial ACL tears recover successfully without surgery when patients adhere to rehabilitation programs. Surgical Treatment Indicated for unstable knees: Surgery may be required if knee stability is significantly compromised. Associated injuries: Meniscus or cartilage damage often requires operative repair along with ACL reconstruction. Athletes needing full stability: Competitive sports participants may undergo surgery for optimal performance. Surgical treatment is generally reserved for severe partial tears or unstable knees. Recovery After Partial ACL Tear Recovery from a partial ACL tear depends on ligament damage extent, age, overall health, and commitment to rehabilitation exercises. Proper care prevents long-term knee issues. Recovery Factors Include Extent of ligament damage: More fiber tears result in a longer healing period and rehabilitation. Age and health: Younger and healthier patients typically regain strength and mobility faster. Consistency with physiotherapy: Regular exercises improve stability and muscle strength effectively. Activity modification: Avoiding high-impact sports ensures safer ligament healing. Recovery timelines may range from 4 to 12 weeks, with consistent therapy being the key to success. Exercises and Rehabilitation for Partial ACL Tear Rehabilitation exercises are essential for restoring knee strength, stability, and flexibility after a partial ACL tear, reducing the risk of re-injury. Common Exercises Include Range-of-motion exercises: Gradual bending and straightening prevent stiffness and promote healing. Strengthening exercises: Quadriceps, hamstrings, and glute muscles support the knee joint. Balance and coordination drills: Enhance stability and prevent future ligament injuries effectively. Functional exercises: Simulate daily and sports movements to regain full knee function. Structured rehabilitation ensures safer recovery and improves long-term knee health after injury. Long-Term Effects of Partial ACL Tear Without Surgery Ignoring a partial ACL tear can lead to chronic instability, recurrent injuries, and degenerative joint changes over time. Potential Complications Chronic knee instability: The knee may repeatedly “give way,” affecting daily activities. Recurrent injury: Unhealed fibers increase the likelihood of further ligament damage. Early-onset arthritis: Poor healing may accelerate cartilage wear and joint degeneration. Reduced mobility:
Best Treatment Options for Posterior Shoulder Dislocation: From Reduction to Surgery

Best Treatment Options for Posterior Shoulder Dislocation: From Reduction to Surgery Posterior shoulder dislocation is a rare but serious medical condition in which the head of the humerus moves backward out of the shoulder socket. Due to subtle clinical signs, posterior shoulder dislocation is often missed during initial examination, leading to delayed treatment and a higher risk of complications. In many cases, Shoulder Dislocation is incorrectly diagnosed as a simple shoulder strain or frozen shoulder, which can worsen joint stability over time. Unlike anterior shoulder dislocation, posterior shoulder dislocation usually occurs due to seizures, electric shock, high-impact trauma, or forceful internal rotation of the arm. Patients with osterior Shoulder Dislocation commonly experience shoulder pain, stiffness, restricted external rotation, and difficulty lifting the arm. Early diagnosis of posterior shoulder dislocation is essential to prevent joint damage, instability, and the risk of recurrent shoulder dislocation. Understanding Posterior Shoulder Dislocation Posterior shoulder dislocation occurs when the humeral head is displaced backward from the glenoid socket. It usually results from seizures, electrical shock, trauma, or forceful internal rotation of the arm. Because symptoms may appear subtle, posterior shoulder dislocation is frequently misdiagnosed as a simple shoulder injury or muscle strain. Common Symptoms Include: Severe shoulder pain and stiffness Limited external rotation Flattened anterior shoulder appearance Early recognition of posterior shoulder dislocation is critical to prevent recurrent shoulder dislocation and cartilage damage. Types of Shoulder Dislocation Understanding shoulder dislocation types helps determine the correct treatment plan. These include anterior, posterior, and inferior dislocations. Each type differs in cause, symptoms, and severity. Proper identification ensures timely shoulder dislocation treatment, reduces complications, and lowers the risk of recurrent shoulder dislocation and long-term joint instability. Anterior shoulder dislocation (most common) Posterior shoulder dislocation (rare but often missed) Inferior shoulder dislocation (luxatio erecta) Diagnosis of Posterior Shoulder Dislocation Shoulder dislocation types include anterior, posterior, and inferior dislocations. Each varies in cause, symptoms, and severity. Correct identification allows timely shoulder dislocation treatment, helps restore joint stability, and reduces pain, complications, and the risk of recurrent shoulder dislocation. Imaging Techniques Used: Standard X-ray (AP view may appear normal) Axillary view X-ray CT scan for bone defects MRI for soft tissue damage Because posterior shoulder dislocation can be overlooked on routine imaging, advanced scans are often required before deciding on treatment. Non-Surgical Treatment Options 1. Closed Reduction Closed reduction is the first-line treatment for acute posterior shoulder dislocation if diagnosed early. This procedure involves gently guiding the dislocated shoulder back into position under sedation or anesthesia. Key points of closed reduction: Best within 24–48 hours of injury Requires experienced orthopedic handling Followed by immobilization After reduction, the shoulder is immobilized using a brace to allow healing and prevent a dislocated shoulder from recurring. 2. Immobilization and Physiotherapy Once the posterior shoulder dislocation is reduced, immobilization is followed by guided physiotherapy. Rehabilitation focuses on: Restoring shoulder mobility Strengthening rotator cuff muscles Preventing recurrent shoulder dislocation This conservative shoulder dislocation treatment works well in first-time, stable cases without bone defects. When Surgery Is Required Surgery becomes necessary when closed reduction fails, the dislocation is old or recurrent, significant bone damage exists, or shoulder instability continues despite proper rehabilitation and conservative shoulder dislocation treatment. Closed reduction fails The dislocation is old or neglected There is recurrent shoulder dislocation Significant bone or cartilage damage exists Delayed treatment of posterior shoulder dislocation increases the risk of chronic pain and joint instability. Shoulder Dislocation Surgery Options 1. Open Reduction Surgery Open reduction is performed when closed reduction is not possible. The surgeon directly visualizes the joint and repositions the humeral head. This type of shoulder dislocation surgery is usually required in locked posterior shoulder dislocation cases. 2. Bone Defect Reconstruction In chronic posterior shoulder dislocation, bone defects (reverse Hill-Sachs lesions) may be present. Surgical reconstruction helps restore joint stability. Common procedures include: Bone grafting Modified McLaughlin procedure Tendon transfer techniques These procedures significantly reduce the risk of recurrent shoulder dislocation. 3. Arthroscopic Shoulder Surgery Minimally invasive arthroscopy is widely used for posterior shoulder dislocation treatment because it allows precise repair through small incisions. This technique reduces pain, limits tissue damage, improves joint visualization, speeds recovery, and helps restore shoulder stability while lowering the risk of recurrent shoulder dislocation. Benefits include: bility while lowering the risk of recurrent shoulder dislocation. Smaller incisions Faster recovery Less post-operative pain Arthroscopy is ideal for patients with soft tissue injuries and instability rather than major bone loss. Recovery After Posterior Shoulder Dislocation Treatment Recovery depends on whether the posterior shoulder dislocation was treated conservatively or surgically. Typical Recovery Timeline: Immobilization: 3–6 weeks Physiotherapy: 6–12 weeks Full activity: 3–6 months Following shoulder dislocation surgery, rehabilitation is crucial to regain strength and prevent another dislocated shoulder. Preventing Recurrent Shoulder Dislocation To avoid recurrence after posterior shoulder dislocation treatment: Follow physiotherapy strictly Avoid early heavy lifting Strengthen shoulder stabilizers Address seizure disorders if present Proper post-treatment care greatly reduces the chances of recurrent shoulder dislocation and long-term complications. FAQs What is posterior shoulder dislocation? Posterior shoulder dislocation occurs when the upper arm bone moves backward out of the shoulder joint. It is less common than other shoulder dislocation types and is often missed during early diagnosis. What causes posterior shoulder dislocation? Posterior shoulder dislocation is commonly caused by seizures, electric shock, high-impact trauma, or forceful internal rotation of the arm. These events push the shoulder backward, leading to joint instability. How is posterior shoulder dislocation diagnosed? Diagnosis of posterior shoulder dislocation requires special X-ray views, CT scan, or MRI. Standard X-rays may not clearly show the injury, which is why osterior Shoulder Dislocation is sometimes overlooked. What are the treatment options for posterior shoulder dislocation? Treatment depends on severity and timing. Options include closed reduction, immobilization, physiotherapy, and in severe or recurrent cases, shoulder dislocation surgery. Can posterior shoulder dislocation happen again? Yes, posterior shoulder dislocation can recur if not treated properly or if rehabilitation is incomplete. Proper shoulder dislocation treatment and muscle strengthening







